Evaluating the Reforms of the Medical-Legal
Process Using the WCIRB Permanent Disability Survey
Table of Contents
I. The California Workers’ Compensation System
Instituted as part of Hiram Johnson’s reforms in 1911, the workers’ compensation system is charged with providing California workers and employers with a no-fault means of resolving claims resulting from on-the-job injuries. In exchange for the certainty of payments for medical, indemnity, and rehabilitation costs, workers waive most of their rights to sue employers. Employers, on the other hand, are provided with a means to spread risk, by having their possible exposure to injury loss capped.
In basic form, a worker enters the workers’ compensation system when he/she is injured. Both the worker and the employer are obligated to report injuries. The worker then may be evaluated by one or more specialists to determine legal issues related to the injury. Specialist exams may either be performed at the request of the worker, the employer, by both (an agreed medical evaluation) or on rare occasions an independent medical evaluation is requested by the Workers’ Compensation Appeals Board (WCAB). An agreement may then be reached on the medical-legal issues, or if the finding is disputed, a variety of judicial and arbitration processes are used to arrive at a settlement. Cases are ultimately settled one of six possible ways:
- Voluntary Payments: The insurer makes voluntary payments and issues are not in dispute.
- Compromise and Release: The employer and worker agree on all disputed issues. The insurer makes payment(s) and the worker, in exchange, releases the insurer from all future obligation.
- Stipulated Award: Similar to Compromise and Release, except that the worker does not release the insurer from all obligation. Usually the stipulation is for future medical benefits.
- Finding and Award: A judge awards the worker a benefit or payment(s).
- Dismissal: A judge dismisses a case, and no award is made. This is largely done in cases where the worker fails to meet a court appearance.
- Take Nothing: A judge rules a claim without merits, and does not award a settlement to the worker.
Of these possible resolution methods, the least demanding on the Division of Workers’ Compensation (DWC) in terms of workload is voluntary payment. The next two methods (Compromise & Release and Stipulated Award) generally place the second least demand on DWC resources solution, while the last three (Finding and Award, Dismissal, and Take Nothing) involve high legal and preparation costs regardless of outcome.
Medical-legal reports are conducted to determine the following issues:
- Worker’s eligibility for benefits
- Ability to return to work
- Permanent and stationary status of the employee’s medical condition
- Existence and extent of permanent disability
- Employee’s preclusion or likely preclusion from engaging in his or her usual occupation
- Extent and scope of medical treatment
- Existence of new and further disability
These reports are conducted at the request of the worker, the employer, and on some occasions at the request of a DWC/WCAB referee/judge.
Under current law, reports are written by the injured worker’s treating physician(s) or a Qualified Medical Evaluator (QME) as approved by the Industrial Medical Council (IMC). QMEs can be acting as an Agreed Medical Evaluator (AME)/Independent Medical Evaluator (IME) agreed upon by both parties or appointed by a judge, a QME chosen by either the employer or the worker in a dispute where the worker is represented by an attorney, or a QME chosen from a panel when the worker is not represented. Prior to the 1993 reforms, the evaluator chosen by parties in a disputed case was not required to be a QME if the worker was represented.
II. Total cost of Medical-Legal Exams
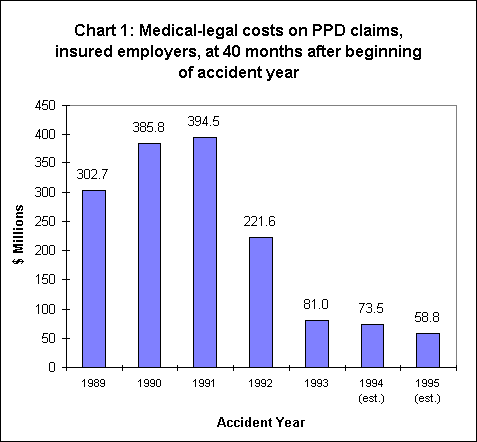
The cost of medical-legal exams on PPD claims has declined considerably since its peak during the 1991 accident year. For the insured community, the total cost of medical-legal exams performed on PPD claims at 40 months after the beginning of the accident year has declined from a high of $394 million for the 1991 accident year to an estimated $59 million for the 1995 accident year. This is a decline of 85 percent in the cost of medical-legal reports and represents a savings of $336 million on the accident year (see Chart 1).
This decline in costs reflects changes in all the components of the cost structure. Consider medical-legal exam costs on PPD claims as composed of the following components:
Total Cost = Number of PPD Claims * Average Cost/Exam * Average Number of Exams/Claim
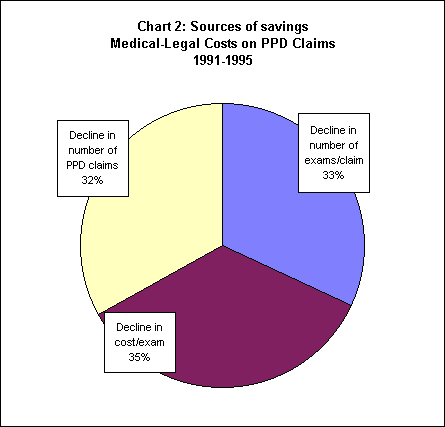
Then, as Chart 2 displays, thirty-two percent of the decline in medical-legal costs can be attributed simply to a decline in the number of PPD claims. Thirty-five percent is due to a decline in the average cost per exam. And the other thirty-three percent of the savings results from a decline in the average number of exams per claim.
The data for this report are drawn from the Workers' Compensation Insurance Rating Bureau's Permanent Disability Survey. The survey and our methodology are describedin Appendix 2.
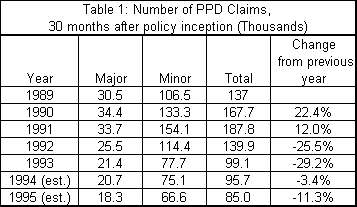
Table 1 shows the number of PPD claims for the 1989 through 1993 accident years based on WCIRB second level individual case reports. Projections of PPD claim levels for the 1994 and 1995 accident years at a similar level of maturity (30 months following the beginning of the policy year) were made by UC DATA for comparison. The frequency of claims is broken down by major and minor disabilities.
The decline in PPD claims is driven by a decline in the number of covered workers, and the number of reported injuries. A substantial portion of the decline in PPD claim frequency may be the result of a steep drop in the number of claims with a psychiatric component, efforts to reduce fraudulent claims, and restrictions on post-termination claims.
As described above, the number of major and minor PPD claims in the system for years 1989 through 1993 was obtained from second level individual case reports. The data from these years have been weighted to reflect the distribution of cases in the second level individual case reports.
Accident year data on the frequency of PPD claims is not available for years following 1993. The WCIRB has discontinued calculating these data. The Rating Bureau feels that the calculation of these data was required by legislation and regulation arising from the 1989 reforms. Since these reforms have been superseded by the 1993 reforms, the Bureau no longer feels compelled to make these calculations. However, this report and the numerous valuable reports issued by the WCIRB are testament to the value of these data. Since most legislative changes are geared to the calendar year, analysis of the impact of these changes is difficult and unreliable when only policy year data is available. The Commission and Department of Insurance should request that the WCIRB continue to calculate accident year injury statistics for use in calculations of frequency and rates by calendar year.
In the absence of accident year data, the frequency of major and minor PPD claims for the 1994 and 1995 accident years is estimated using Division of Labor Statistics and Research (DLSE) data on the frequency of disabling injuries for 1993, 1994, and 1995. The ratio of 1994 to 1993 and 1995 to 1993 disabling injuries was applied to the frequency of 1993 PPD claims as reported by the WCIRB from second level individual case reports to develop estimates of 1994 and 1995 PPD claims. Since the frequency of PPD claims has been falling more rapidly than the frequency of disabling injuries, this may slightly overestimate the number of PPD claims for 1994 and 1995. As an example, a similar procedure was used in our previous report to estimate the number of PPD claims for 1993 and 1994. This estimate (104,000 for 1993) overestimated the actual number by approximately 5%.
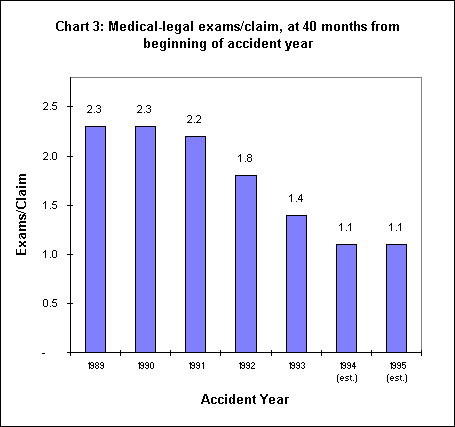
Chart 3 illustrates the decline in the number of exams per claim. The 53 percent decline since 1989 is in part a reflection of changes made that were meant to reduce the "dueling docs" syndrome. Other changes include reestablishing the role of the treating physician and establishing the treating physician’s findings as presumed correct except with a preponderance of evidence, limiting the number of exams allowed per specialty in litigated cases, cover-age of all issues in a single "comprehensive" evaluation, actions against mills, and, as noted below, an aggressive efforts against fraud and to reduce psychiatric exams.
The number of exams per claim at 40 months from the beginning of the accident year for the 1989-1993 accident years were obtained from the survey.
Projections for the estimated number of exams per claim for the 1994 accident year were obtained by calculating the historic growth rate between 28 and 40 months in the average number of exams per claim. This rate was then applied to the average number of exams per claim obtained from the survey at 28 months after the beginning of the accident year to obtain an estimate for expected average number of claims at 40 months.
1995 projections were obtained by first calculating a ratio of 1994 to 1995 average number of exams per claim using comparable claims (claims incepting from January through July, and valued at 16 months from the beginning of the accident year). This ratio was then applied to the estimate of the 1994 exams per claim projection for 40 months to obtain an estimate of exams per claim at 40 months for the 1995 accident year claims.
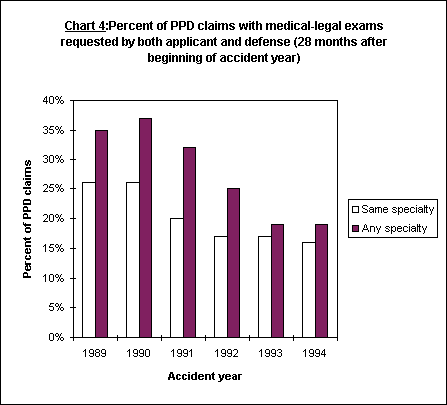
Reforms in 1989 and 1993 attempted to reduce the number of medical-legal reports resulting from applicants and defense attorneys bolstering cases with multiple reports by forensic doctors, often referred to as the "dueling docs" phenomenon. The survey data indicate that these efforts have been successful. The percent of PPD claims with applicant and defense medical-legal exams by doctors in the same specialty has declined by just over 1/3 from the 1989 accident year to the 1993 and 1994 accident years. The percent of claims with both applicant and defense exam requests, regardless of the specialty, declined over the same period by nearly half (48%). These data are shown in Chart 4.
C) Impact of Treating Physician
The reform legislation reestablished the role of the treating physician in writing evaluations of all medical issues concerning compensation and writing comprehensive medical-legal reports beginning in 1994. When treating physicians evaluations, paid under the treatment fee schedule, replace QME evaluations, the average number of medical-legal reports per claim is reduced. Also, the legal standing of the treating physician acts to discourage either party from disputing issues and obtaining a medical-legal report.
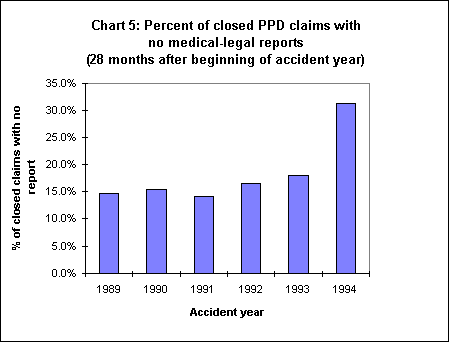
We analyzed this issue by calculating the percentage of PPD claims resolved without any reported medical-legal exams. This was done for the 1989-94 accident years and was calculated for claims resolved within 28 months of the beginning of the accident year. These data are shown in Chart 5.
The portion of claims closing with no recorded exams remained steady at approximately 14-16% from 1989-93. For the 1994 accident year, the portion of claims with no exams doubled to over 31%. Alternately, specifying the time period as 28 months after the date of injury gave identical results. It seems reasonable to attribute much if not most of this change to the reintroduction of the role of the treating physician. When the evaluation upon which the case is resolved is a treatment report that would have been produced and reimbursed in the usual process of patient care, then this change represents a pure cost savings on medical-legal costs. It does not, however, answer the question of the impact of the quality of these reports on other aspects of case resolution or the fairness, accuracy, or precision of the settlement.
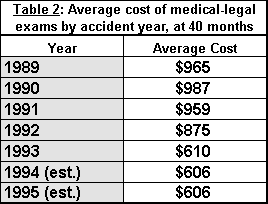
As seen in Table 2, the average cost per exam has declined from a high of $987 for the 1990 accident year claims to the current estimate of $518 for the 1995 accident year claims. This improvement in exam cost is driven by at least three important changes. First, the Medical-Legal Fee Schedule underwent several revisions. The fee schedule in effect after August 3, 1993 attempted to substantially reduce the cost of exams by restructuring the schedule and reducing the level of acceptable charges. The schedule under which fees are set is determined by the service date of exams rather than the date of injury. Most 1993, and all 1994 and 1995 exams, have service dates in the period following August 3, 1993 when the lowest fee schedule amounts were in effect. Only a fraction of 1991 and 1992 accident year claims have exams in this period, and no exams in the WCIRB PD Survey of the 1989 and 1990 accident years fell in this period.
Second, the average cost of exams is also determined by the mix of specialties of the reporting doctors. Some provider specialties have higher than average costs. The larger the proportion of costly exams, obviously, the higher the average cost of the claim. Psychiatric exams are substantially more expensive than exams by other specialties. The steep decline in the number of psychiatric exams is responsible for 19 percent of the decline in the average cost of all exams. If the proportion of exams that were psychiatric had remained steady at the 1991 accident year level, the average cost of medical-legal exams would have been $60 greater for the 1994 accident year.
Third, for injuries occurring after January 1, 1994, reform legislation reestablished the role of the treating physician in writing medical-legal reports. This issue is covered in the following section.
For survey years 1989 through 1993, average cost per exam was obtainable from the survey itself, as all claims have been observed for 40 months from the beginning of the accident year. For 1994 and 1995 claims, all exams occur in the period after the least costly fee schedule went into effect. Accordingly, we assumed the average cost per exam would remain constant at the current level. It should be noted that analysis across all years, controlling for the fee schedule in effect, did not reveal a change in the average cost of exams as the claims matured from 16 months to up to 64 months.
However, it should also be noted that the claims for the 1995 accident year had on average only 13 months of maturity before they were surveyed by the WCIRB. While claims from 1989 to 1993 did not show changes in average cost over time, the reintroduction of the treating physician may change this pattern for injuries after 1/1/94. If treating physician reports are substantially less costly and they represent a higher proportion of exams done within 16 or 28 months after the beginning of the accident year, the average cost estimates in Table 2 would underestimate the average cost of medical-legal reports over the life of the claim for accident years 1994 and later. The special panels drawn for 1994 and 1995 are too small for complete analysis of this issue.
B) Impact of Treating Physician on Average Cost
The reintroduction of the treating physician role in the medical-legal process affects the average cost of medical-legal reports in two ways.
1) When billed as a medical-legal report, the fee schedule sets reimbursement rates for treating physicians at 80% of those set for forensic specialists who are not also the treating physician.
2) Treating physician reports, paid under the Official Medical Fee Schedule, may be incorrectly recorded on the WCIRB survey as medical-legal exams, especially reports done shortly after the new regulations went into effect. This would lead our figures to underestimate the average cost of medical-legal reports.
The WCIRB PD Survey does not record the nature of the report writing physician other than to identify the report as Applicant, Defense, or AME. However, UC DATA examined a sample of several hundred files at the Workers’ Compensation Appeals Board with dates of injury in 1994 that closed prior to Feb. 1, 1997. As indicated in Table 3, of the medical-legal reports filed for resolution of permanent disability issues on these claims, 36% were by treating physicians. Thus, at a 20% discount, the treating physician scheduled savings would account for, at most, only a third of the reduction in the average cost per exam experienced between 1993 and 1994.
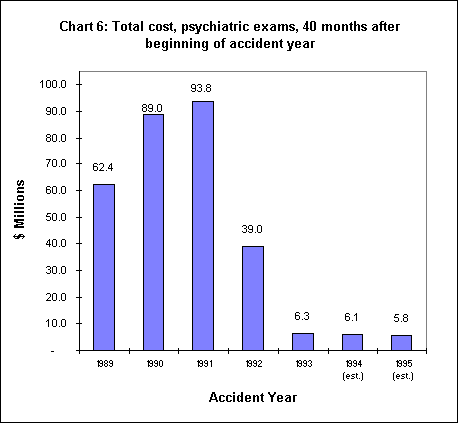
Much of the decline in the average number and the average cost of medical-legal exams per claim is the result of reductions in the number and cost of psychiatric claims. Psychiatric claims were subject to specific legislation that impacted these claims separately from other types of claims.
As shown in Chart 6, the total cost of psychiatric exams has declined from a high for the 1991 accident year of $93.8 million to an estimated low of $5.8 million in 1995. This represents a savings of $88 million, or 94 percent, in the cost of psychiatric related medical-legal exams. This reduction accounts for 26% of the overall reduction in all medical-legal costs between the 1991 and 1995 accident years.
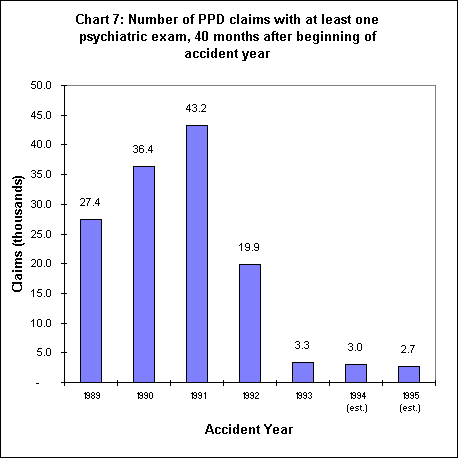
The decline in the total cost of psychiatric exams is due to both a drop in the number of psychiatric claims and a decline in the cost per exam. As shown in Chart 7, the number of psychiatric claims (defined here as PPD claims with at least one psychiatric medical-legal exam) has declined by 93 percent between accident year 1991 and 1994. It should be noted that for injuries occurring after January 1, 1994, the employer is required to pay for only a single physician (or single physician for each side) to evaluate all open issues. Consequently, for 1994 and later injuries, the survey may no longer allow us to determine cases with a psychiatric component. This will often be obscured when the evaluating physician chosen is from another specialty.
B) Frequency of Psychiatric Claims
Part of this decline in number of psychiatric exams is driven by the overall decline in all types of PPD claims. In addition, as Table 3 indicates, the decline is driven by factors specific to psychiatric claims that reduced the portion of PPD claims that have a psychiatric component. Anti-fraud efforts, crackdowns on "mills," and similar efforts may be the most important factors in the declining frequency of psychiatric claims. Limits on post-termination stress claims introduced in 1993 and improvements in the California economy that reduced mass layoffs may also have played a role. The number of psychiatric exams per claim peaked in the period from 1990 through the first six months of 1991, even after passage of the Margolin-Bill Greene Workers' Compensation Act of 1989, which attempted to narrow the scope of compensability for psychiatric conditions, and went into effect for injuries occurring on or after January 1, 1990.
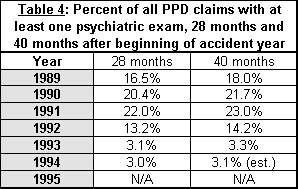
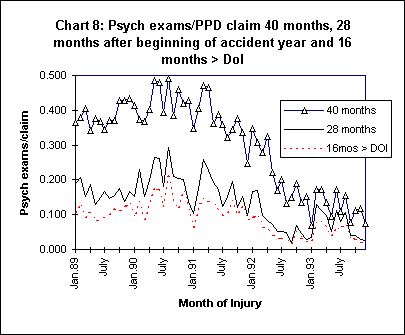
A second bill attempting to limit the number of psychiatric claims, AB 971, went into effect in July, 1991. A noticeable decline in psychiatric exams per claim occurred in mid-1991, but this decline largely predated the implementation of AB 971, beginning in April and May of 1991. This decline in psychiatric exams per claim beginning in mid-1991 accelerated in 1992, and continued into 1993. Further legislation requiring that work be the "predominant" cause of a psychiatric complaint for injuries occurring on or after July 16, 1993 has not drastically accelerated this decline in psychiatric claims in data from 1994 and 1995.
Between 1991 and 1994, more than one-third (34%) of the reduction in the average number of
medical-legal exams per PPD claim is a result of a drop of 84% in the average number of psychiatric exams per PPD claim.
Unlike PPD claims in general, the recent decline in total medical-legal costs on psychiatric claims is not due to a reduction in the average number of psychiatric exams per psychiatric claim. Though the 1994 and 1995 samples are small and not yet complete for 40 months, indications are that the average number of psychiatric exams on psychiatric claims has not declined appreciably since 1992. The number of psychiatric exams per psychiatric claim, when assessed at 16 months after the beginning of the accident year, has remained relatively constant at approximately 1.3-1.5 exams on each claim. Similarly, at 28 months, 1993 and 1994 psychiatric claims show little difference, on average, in the number of psychiatric exams per claim than those in the previous year.
C) Source of Request for Psychiatric Exams
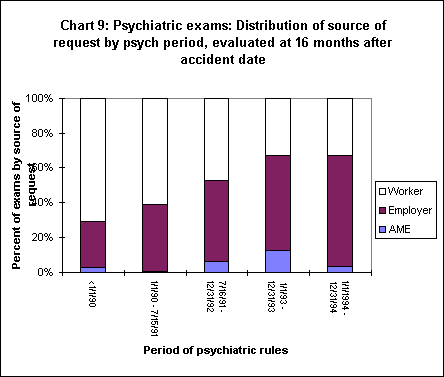
It is interesting to note that the rise in the proportion of all claims with psychiatric exams from 1989-91 was accompanied by only a small rise in the frequency of requests by workers. Chart 9 shows the distribution of exams by the source of request in each of five periods. For this purpose claims were evaluated at 16 months after the accident date.
Requests by employers for psychiatric exams rose more rapidly after 1989 than requests by workers. Moreover, they declined less steeply after the reforms that went into effect in mid 1991. Consequently, as indicated in chart 9, employers have replaced workers as the predominate source of requests for these exams. However, the dramatic decline in the number of psychiatric exams means that these requests are occurring on a relatively small number of claims and the distribution in the sample is likely to be subject to a good deal of variance.
VII. Adjudication and Claims Resolution
A) Improvement on represented claims
In this section of the report we use claims that have been resolved within 40 months and 28 months after the beginning of the accident year to further analyze trends in the number of reports requested per claim.
 The
choice to base this comparison on resolved claims was done to avoid the possibility
that reforms sped up or slowed down the timing of exams on claims. For example,
suppose the number of exams stayed the same, but they occurred earlier in the
life of a claim. If we valued all claims at similar points in time, it would
appear the number of exams was increasing. We avoid that problem in this analysis
by only looking at claims that have been resolved. The number of exams which
will occur is certain on closed claims.
The
choice to base this comparison on resolved claims was done to avoid the possibility
that reforms sped up or slowed down the timing of exams on claims. For example,
suppose the number of exams stayed the same, but they occurred earlier in the
life of a claim. If we valued all claims at similar points in time, it would
appear the number of exams was increasing. We avoid that problem in this analysis
by only looking at claims that have been resolved. The number of exams which
will occur is certain on closed claims.
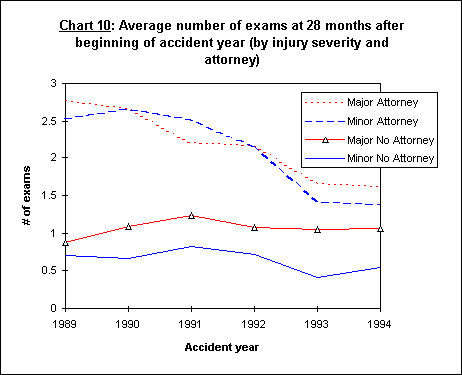
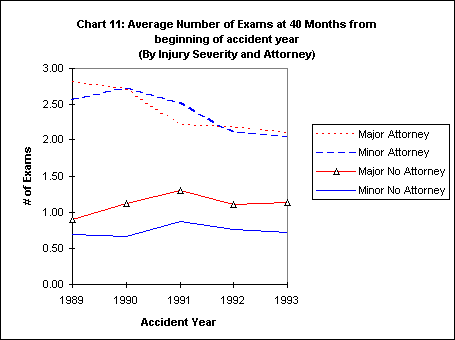
When these data are further disaggregated, it is clear that the decline in the number of exams is being driven primarily by the improvement on the represented claims. Chart 10 and Chart 11 show the data disaggregated by represented/unrepresented and major/minor injuries.
Regardless of whether the injury is major or minor, the represented cases in this period have had more exams than the unrepresented. This gap is, however, narrowing. While the frequency of exams on unrepresented claims has changed little, the change on represented cases has been substantial.
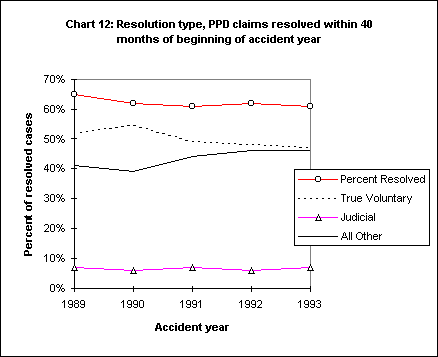
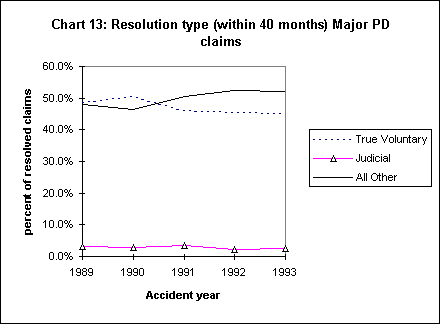
The introduction of mandatory settlement conferences (MSC) was meant to reduce the need for hearings and decisions, and to speed the resolution of cases. Have these new mechanisms accomplished these goals? The data from the WCIRB survey suggest the answer is no. Have the resolution mechanisms had unintended impacts on the frequency of medical-legal reports? The data offer some support that they have, albeit relatively weak support. Charts 12, 13, and 14 show the resolution of cases at 40 months from the beginning of the accident year.
These data reveal a decline in the percentage of cases where a voluntary agreement was reached without intervention by the DWC/WCAB, and an increase in the percentage of cases where the DWC has been involved. This is true for both major and minor injuries. Each of these subgroups exhibits the same pattern of little to no change in the rate of judicial settlements and a rise in the proportion of claims using dispute mechanisms. This is occurring despite the decline in stress claims, rules against post-termination claims, and other legislative changes that would be expected to have their greatest impact on the most disputed and difficult to resolve claims.
While the number of PPD claims has declined, the likelihood of DWC/WCAB intervention to resolve claims has actually increased, possibly as a result of the new resolution methods. Instead of reaching voluntary settlements that do not involve active involvement by the DWC/WCAB, parties are increasingly using one or more dispute resolution methods.
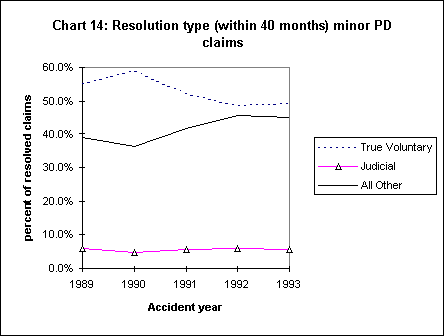
Some claims that would have been settled voluntarily are now using at least one dispute resolution mechanism. The movement of cases from voluntary settlement to dispute mechanisms has not been accompanied by a reduction in the need for formal decisions to resolve claims. The proportion of cases settled through formal hearings has not changed.
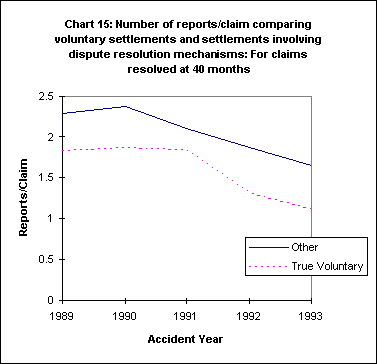
These resolution methods may have had unintended impacts on the frequency of medical-legal reports. While the frequency of reports done on claims resolved within 28 months or 40 months has declined, the apparent movement of cases from voluntary settlement to other resolution mechanisms may be attenuating some of the savings to the system. Claims using one or more resolution methods average 15-40% more medical-legal exams (see Chart 15). This gap has widened even as claims have apparently moved from the voluntary processes into dispute resolution.
There has been no significant improvement in the rate at which cases close. Hazard analysis was used to attempt to obtain a measure of the system’s ability to process claims, independent of the type of claim, level of attorney involvement, etc. Based upon this analysis conducted as in our previous report, there are no significant differences in the time taken to case resolution in the 1990s. The system remains stubbornly resistant to attempts to speed up the resolution process. After controlling for injury severity, the number and type of specialty exams, and presence of employee legal representation, there is no statistically significant improvement in time to case resolution between 1990 and 1993, despite the variety of reforms which have been enacted during that time. Indeed, the only statistical difference between any particular accident years that we find is that cases following 1989 appear to be resolved more slowly than cases arising during the 1989 accident year. If anything, the 1993 claims show a disturbing trend towards slightly longer duration. The key will be when data on a full panel are available for 1994. This will allow hazard analysis to be performed for the first time on data for years following the 1993 reforms.
The 1996 report by the Commission evaluating the reforms to the medical-legal process found dramatic improvements since 1989 in the cost and frequency of medical-legal reports. Much of that analysis required projections for the 1993 and 1994 accident years. The current report, using more recent data, confirms those savings and the accuracy of the projections.
These more recent data also suggest that the substantial savings, especially for the 1993 and 1994 accident years, continue into the 1995 accident year. The 1996 report found that a substantial source of these savings resulted from changes in the Medical-Legal Fee Schedule and the decline in psychiatric exams and claims. These trends continue to be demonstrated in the 1997 report’s findings.
In addition, data for the 1994 and 1995 accident years suggests an additional source of major cost savings, the reintroduction of the role of the treating physician. This legislative change is likely responsible for a substantial portion of the decline in the average cost and frequency of medical-legal reports on claims occurring after January 1, 1994. However, these data for 1994 and 1995 injuries come from special panels that are smaller than the full panels drawn for 1989-1993. The survey conducted during the current year, with a full panel of 3500 claims for 1994, will be important in analyzing this trend.
Finally, analysis of the time required to resolve PPD claims continues to demonstrate the resistance of the system to more rapid claim resolution. This is especially troublesome in view of the decline in the number of PPD claims, which should have reduced workloads and speeded resolution. The full 1994 panel, available late in 1997, will be critical to determining if the 1993 reforms have finally been able to achieve the goal of speeding up the claim resolution process.
Appendix 1: Summary of Legislative and Regulatory Changes
The 1989 and 1993 workers’ compensation reforms were intended to decrease system costs and the amount of time needed to settle cases. Many of these reforms were meant to directly or indirectly affect the medical-legal process.
A. Recent Legislation Affecting the Cost of Medical-Legal Evaluations
Legislation has changed the amount rebuttably presumed reasonable for medical-legal reports. Prior to 4/3/93, these were determined by specialty (Orthopedic, Neurological, Internal/Cardiology, Psychiatric, and All Other). After that time, the specialty was no longer a determinant, but the reports were separated into the following four categories:
Follow-up (ML101): Includes examination of patient within one year of initial evaluation.
Basic (ML102): All evaluations, other than Supplemental, Complex, or Extraordinary.
Complex (ML103): Includes three or more of following:
- 2 or more hours physician face to face with patient;
- 2 or more hours of record review by the physician;
- 2 or more hours of medical research by physician;
- addressing the issue of medical causation;
- addressing the issue of apportionment
- monitoring after toxic exposure
Extraordinary (ML104): Used in place of ML101-103 where significantly more time is needed than the code allows. (see Title 8, CCR 9795 for conditions)
A premium above the fee schedule amount was allowed where an interpreter was necessary or the evaluator was acting as an "Agreed Medical Evaluator" (AME) code 94, multiplier 1.25.
Reports by a Primary Treating Physician under the Medical-Legal Fee Schedule, have code 92 attached and a multiplier of 0.8
Table A1: Amounts presumed reasonable: medical-legal reports
| ORTHO | CARDIO/
INTERN |
NEURO | PSYCH | OTHER | |
| 11/1/86
to
10/1/87 |
870 |
891 |
742 |
1147 |
650 |
| 11/1/87 to 10/31/88 |
943 |
982 |
883 |
1217 |
762 |
| 11/1/88 to 10/31/89 |
1001 |
1020 |
893 |
1275 |
962 |
| 11/1/89 to 12/31/89 |
1025 |
1050 |
900 |
1400 |
915 |
| 1/1/90 to 6/30/92 |
984 |
995 |
881 |
1279 |
866 |
| 7/1/92 to 4/2/93 |
1070 |
1121 |
994 |
1427 |
1019 |
| 4/3/93
to
8/2/93 |
no schedule |
||||
| after 8/3/93 |
$500 basic, $750 complex, 200/hr extraordinary, $250 follow-up |
||||
These changes would be expected to impact the cost of medical-legal reports. The minor adjustments to the fee schedule made prior to 8/3/93 are likely to affect only the portion of exams whose cost was at or near the rebuttable maximum. Exams with costs much above or below the fee schedule targets would likely be unaffected by these small changes.
The very large change to the maximums introduced for exams conducted on or after 8/3/93 should affect a much wider range of exams, and would be expected to reduce costs more dramatically than previous reductions. Again, exams whose costs were considerably below the new maximum would presumably not be affected.
The average cost of medical-legal reports can also be affected by the mix of reports. A decrease in the relative frequency of reports by a more expensive specialty could reduce the average cost of reports even while all specialties individually were more expensive. For example, if the frequency of psychiatric reports (the most expensive reports) declined enough, that alone could reduce average cost of all reports even if all specialties, including psychiatric, had increased in cost.
Alternatively, if reports requested by employers were less expensive on the average than those requested by workers (as we will discuss below), a decrease in the frequency of reports requested by employers relative to workers would appear to drive the cost of the average report higher. This argues for an effort to disaggregate the analysis of medical-legal reports by studying them by both specialty and source of request.
B. Recent Legislation Affecting the Frequency of Medical-Legal Reports
1989 Legislation:
The Margolin bill created the Qualified Medical Evaluator (QME) and alternative dispute resolution mechanisms. In addition, the statute limited each party to a single medical-legal report on any issue by each appropriate specialty or subspecialty. Chapter 892 also prohibits admission into evidence of any medical opinion, other than a report from the treating physician, that was obtained before the service of the assessment by the Agreed or Qualified Medical Evaluator.
1993 Legislation:
AB 110 (Peace) 1993 Stat. Chap. 121, effective July 16, 1993 made numerous changes to the process of selecting medical evaluators, which could be expected to reduce the number of reports. Chapter 121 allows the treating physician, who is primarily responsible for the care of the injured worker, to write a comprehensive medical-legal evaluation if a dispute develops. Legislation in 1989 had restricted the use of the treating physician by requiring separate report(s) by Qualified Medical Evaluators.
Chapter 121 also provided that where an additional comprehensive exam is obtained, the findings of the treating physician are presumed to be correct except with a preponderance of evidence, unless both parties elect QMEs. This encourages one or both parties to avoid seeking additional evaluations.
Other legislation restricted medical-legal examinations during the first sixty days, except at the request of the employer, and limited the employer’s financial responsibility to a single comprehensive evaluation covering all issues.
C. Recent Legislation Affecting the Frequency of Psychiatric Evaluations
Several legislative changes were expected to reduce the frequency of psychiatric evaluations by restricting the range of psychiatric injuries considered compensable. The changes modified evidentiary rules, imposing a "preponderance of evidence" requirement. A series of changes increased, over time, the degree to which the cause of the injury or illness had to be related to employment.
Assuming that the proportion of psychiatric injuries/illnesses remained steady relative to other injuries in the compensation system, these restrictions should eliminate a number of these injuries from compensability, because the psychiatric component fails to meet the threshold conditions for compensability. However, it could be argued that higher standards of proof lead to the need for more evaluations to establish whether the threshold conditions have been exceeded.
1989 Legislation:
The Margolin-Bill Greene Workers’ Compensation Reform Act of 1989 made changes in the treatment of psychiatric injuries, effective for injuries that occur on or after January 1, 1990. Chapter 892 narrowed the scope of compensability for psychiatric conditions by imposing a requirement that the employee demonstrate industrial causation by a preponderance of the evidence. Under prior law, "substantially in the record as a whole" was the sole evidentiary standard for all workers’ compensation issues. Chapter 892 further required that at least ten percent of the causation of a psychiatric condition be attributable to "actual" employment factors before the employee was eligible for benefits. This legislation also included specific language identifying the "intent of the legislature in enacting this section to establish a new and higher threshold of compensibility for psychiatric injuries."
1991 Legislation:
AB 971 (Peace), effective July 1991, made additional changes by applying a further restriction denying recovery for those psychiatric injuries resulting from regular and routine employment unless the employee has worked for that employer for at least six months.
1993 Legislation:
SB 223 (Lockyer), effective for injuries occurring on or after July 16, 1993, changed the causation standard on psychological injuries to require that actual events of employment must be predominant as to all causes combined. However, if the psychiatric injury results from a violent act or from direct exposure to a violent act, the employee is required to prove by a preponderance of the evidence that actual events of employment were a substantial cause of the injury. Cal. Lab. Code #3208.3(b)(3) (amended by Chapter 1242) defines substantial cause as at least 35-40%. Chapter 1242 also provided that psychiatric injuries are not compensable if substantially caused by a lawful, nondiscriminatory, good-faith personnel action. Further restrictions were also placed on recovery for psychiatric injuries following notice of termination of employment or layoff. The injury must have occurred prior to the time of notice of termination and one or more of the following conditions must exist: 1) sudden and extraordinary events of employment caused the injury; 2) the employer had notice of the injury prior to notice of termination or layoff; 3) employment records contain evidence of previous treatment of the psychiatric injury; 4) a finding of sexual harassment; or 5) evidence that injury occurred after notice of termination or layoff, but prior to the effective date of the termination or layoff.
D. Recent Legislation Affecting the Outcomes of the Medical-Legal Decision Process for Workers
Legislative changes can be expected to change outcome measures of the decision-making process by affecting the disability measurement process. The determination of permanent disability under the statutes and regulations guiding the California system is at best imprecise. This has led to numerous calls to change the way in which we determine permanent disability in our state. Different doctors can give very different evaluations to the same patient.
Doctors having "conservative" and "liberal" interpretations of the level of disability are to some extent known to informed parties. Informed parties are individuals or entities that participate in the system on a frequent basis, for example, employers, insurers, or attorneys. Workers would not be expected to know the biases of doctors since they participate once or at most infrequently. Two well-informed parties could be expected on average to reach unbiased decisions given equal levels of knowledge in choosing their experts. Workers, acting alone, might not be expected to reach a similarly unbiased outcome. Rather, their PPD awards would be expected to be biased downward if information about the evaluating doctors’ interpretation is unknown to the worker and the selection is made by an informed party.
1989 Legislation:
Chapter 892 required that a notice be included with an injured worker’s final payment of temporary disability stating the employer’s position with respect to the employee’s eligibility for permanent disability compensation. Alternate procedures for resolving medical disputes were established dependent upon whether the employee was represented by an attorney.
If an employee was not represented by an attorney, Chapter 892 prohibited the employer from obtaining an agreement on the selection of a medical evaluator. Instead, the statute required that in the event of a medical dispute with an unrepresented employee, the employer must request that the Medical Director assign a panel of three Qualified Medical Evaluators from which the employee can make a selection. This eliminated the prior common practice where the injured worker was given a medical evaluation by a doctor suggested or assigned by the employer’s representative.
E. Recent Legislation Affecting the Time to Resolution
1989 Legislation:
The 1989 reform introduced new mechanisms for resolving disputes. AB 276 provided for a mandatory settlement conference conducted by a referee not less than ten days, nor more than thirty days, after the filing for adjudication. If the settlement conference does not resolve the dispute, the regular hearing will be held within seventy-five days of the filing of the application.
If an injured employee is represented by an attorney, AB 276 requires arbitration in disputes over insurance coverage and rights of contribution. Beginning 1/1/91, arbitration will be required in cases of permanent disability when there is a low percentage of disability and the case cannot be heard within 110 to 150 days of the filing of the application for adjudication.
The introduction of arbitration and mandatory settlement conferences (MSC) were meant to reduce the need for hearings and decisions and to speed the resolution of cases.
Appendix 2. Data and Methodology
Data for this analysis come from the WCIRB Permanent Disability Survey. The survey summarizes accident claim activity, including such measures as the degree of impairment, the type and cost of specialty exams, whether the case was settled and, if so, what settlement method was employed.
Because accident claims are collected as part of an insurance policy, claims cannot be sampled directly. Instead, the WCIRB collects all policies incepting on or after July of the year prior to the accident year through July of the accident year. Using second level case reports, which value claims at 30 month after the beginning of the policy year, the WCIRB identifies accidents:
- with dates of injury in the targeted accident year
- defined as permanent disability claims
Individual claims are stratified by injury severity based on second level individual case reports submitted to the WCIRB. Claims with estimates of permanent disability equal to or greater than 25 percent are considered "major" disabilities, while claims with ratings under 25 percent are considered "minor" disabilities. A stratified random sample of 3,500 permanent disability claims is drawn from all Permanent Partial Disability (PPD) claims on a selected subset of policies, with 1,500 claims coming from the "major" disabilities, and 2,000 claims coming from the "minor" disabilities. This survey has been conducted on claims from the 1989 through 1993 accident years.
The sampling scheme is intentionally designed to oversample "major" disability cases. In reality, only approximately one-fifth of all cases are "major" when evaluated at thirty months after policy inception. Oversampling these "major" cases allows enough data to be gathered so that separate inferences can be drawn about this relatively small population. One negative consequence of this oversampling, however, is that the data necessary to "re-weight" the survey sample population back to the relative distribution of major/minor injuries in the full population of injured workers has to be inferred for the 1994 and 1995 accident years. Weights are available for the 1989-1993 years, but weights for the 1994 and 1995 years were calculated based on estimates of the distribution of major and minor injuries at 30 months after the beginning of the policy year.
These sampled accident claims are re-examined at 52 and again at 64 months following the start of the target year to determine whether claims have been resolved or otherwise changed. At the present time, complete 64 month data exists only for the target years 1989-91.
The data available for the 1994 and 1995 accident years come from "special panels." These were drawn at 28 months and 16 months, respectively, from the beginning of the accident year. Both of these special panels consist of only 350 claims. As a result, variances for all estimates made for these years will be much wider than for the earlier target years.
In addition, because of the different "maturity" times by target year, this analysis is forced to limit comparisons between years by different degrees of case maturity. For example, 1993 claims can be compared at 40 months to 1992 and earlier claims. However, claims for 1993 can only be compared to those for 1994 at 28 months, and to claims for 1995 at 16 months.
The "final" word on the effects of reforms upon the workers’ compensation system through the target year 1994 will therefore have to wait for the third report which will be collected in April 1999 and available in early 2000.
The weights for individual claims for the major and minor strata were not available from the WCIRB. The Rating Bureau creates the weights by evaluating the claims at 30 months after policy inception based on the Unit Statistical Report, second level case reports. We are required to use the PD level reported on the Permanent Disability Survey. These data are from claims when they are several months more mature than thirty months. These two data sources are likely to be very close, but not exactly the same. For future efforts, we will try to obtain the actual weights used by the WCIRB.
In most situations the analysis is done using data available on cases 28 and 40 months after the beginning of the accident year. This allows us to compare data across accident years at similar points in the average maturity of claims. It should be noted that claims occurring on January 1st will have 12 months more activity than claims for accidents occurring on December 31st of the same accident year. Consequently, in some situations we use the actual maturity of the claims in months since the date of injury. This is done, for example, with the analysis of time to resolution and the incidence of psychiatric exams.
Revised July 1997

