CHSWC Report on the Division of Workers’ Compensation Audit Function
Legislative Request for Study of Audit
Function
Project Methodology
Project Organization
Focus
Meetings with the Workers’ Compensation Community
Survey of Audit Programs in Other States
Analyses of Data
Comments on the initial draft report
Overview
Scope of Audit Function
Audit Process
Audit Methodology
Audit Subject Selection Process
Mix of Audit Types
Types of Penalties Cited
Penalty Structure
Determining ‘Compensation
Due’
Definition of ‘Compensation Due’
Statutory changes in payment rates
Calculation of Benefits
Benefit Notice Program
System Performance Measures
Audit Function Administration
Audit Unit Workload
Audit Unit Staffing
Audit Unit Statutory Requirements
Observations by Audit Unit Staff
RecommendationsOverview
Audit Function Recommendations
Improve audit function administration
Increase incentives for timely and accurate delivery of
benefits
Improve targeting of poor performers
Revise Audit Process
Overview of Proposed Audit Process
Highlights of Proposed Changes
Scope of Audit Function
Audit Procedure
Profile Audit Review (PAR)
Full Compliance Audit
Target Audits
Audit Sample Selection Process
PAR Sample Selection Process
FCA Sample Selection process
Passing/Failing a PAR Audit
Passing/Failing a FCA Audit
Passing/Failing a Targeted Audit
Ranking of Locations According to Performance
Other Workers’ Compensation System Recommendations
Pay all benefits at a single weekly
rate
Simplify Permanent Disability Calculations
Improve Benefit Notice Program<
CHSWC Benefit Notice Project
Change Mechanism for Commission Funding
Implementing the New Audit SystemAction Steps
Staffing Required for Revised Audit Process
Appendices
Appendix A Labor Code Sections 129
and 129.5
Appendix B Legislative Request for Study of Audit
Function
Appendix C Insurance Code Sections 790-790.10
Appendix D CHSWC Audit Study Advisory Committee
Appendix E Research Questions for Audit Study
Appendix F Audit Programs in Other States
Appendix G Description of Current Audit Selection
Process
Appendix H Audit Penalties 1995-1997*
Appendix I Complexity of the Benefit Delivery Process
Appendix J Analysis of ‘Compensation Due’ for
1997
Appendix K Evaluation of Data and Goals of the Audit
Unit
Appendix L Activities of the Audit Unit
Appendix M Analysis of the Fair Claims Settlement
Practices Act
Appendix N Discussion of Current Audit Targeting
Process
Appendix O Discussion of Eliminating Administrative
Penalties at the PAR Level
Appendix P PAR and FCA Performance Standards
Appendix Q Proposed Administrative Penalty Structure
Appendix R Impact of Single Rate Payments
Appendix S Proposed Legislation
Commission on Health and Safety and Workers’ Compensation
CHSWC Report on the
Division of Workers’ Compensation Audit Function
The 1989 California workers’ compensation reform legislation established an audit function within the Division of Workers’ Compensation (DWC) of the Department of Industrial Relations (DIR).
The intent of the audit function is to monitor the performance of workers’ compensation insurers, self-insured employers, and third-party administrators to ensure that industrially-injured workers are receiving proper benefits in a timely manner.
The duties and responsibilities of the DWC administrative director with respect to audits of workers’ compensation insurers, self-insured employers, and third-party administrators are specified in Sections 129 and 129.5 of the California Labor Code, shown in Appendix A.
The purpose of the audit function is to provide incentives for the prompt and accurate delivery of workers’ compensation benefits to industrially-injured workers and to identify and bring into compliance those insurers, third-party administrators, and self-insured employers who do not deliver benefits in a timely and accurate manner. The audit function, together with a Benefit Notice program, could also provide indicators of potential system and operational problems that need addressing.
Legislative Request for Study of Audit Function
In April 1998, the Honorable Hilda L. Solis, Chair of the Senate Industrial Relations Committee, and the Honorable Liz Figueroa, Chair of the Assembly Insurance Committee, jointly requested that the Commission undertake an evaluation of the effectiveness of the audit function of the Division of Workers’ Compensation. The letter from the Legislative committees to CHSWC Chairman Tom Rankin is shown in Appendix B.
The Legislature requested that the Commission work to develop recommendations:
- To make the DWC Audit program more effective,
- To determine whether or not the program is adequately staffed,
- To determine whether or not the penalty levels are adequate and/or appropriate to deter violations,
- To make the $100,000 civil penalty for a pattern and practice of poor claims administration more effective, and
- To consider whether or not the unfair claims settlements practice act (Insurance Code Section 790.03) should apply to workers’ compensation. [See Appendix C for Insurance Code Sections 790-790.10]
This legislative initiative was in part a response to considerable concern raised by some members of the workers compensation community. These concerns focused on the results of recent annual audits that showed substantial numbers of violations and found what many felt were excessive levels of unpaid compensation. Some observers also interpreted these data, when extrapolated to the entire population of claims locations, to indicate a trend toward poor performance in the delivery of benefits to injured workers.
A project team, comprised of CHSWC staff and independent researchers, was formed to carry out the Legislative Committees’ request.
CHSWC also established an Audit Review Advisory Committee, comprised of representatives from throughout the workers’ compensation community, to assist the project team in this endeavor. Appendix D contains a listing of the names and organizational affiliations of the members of CHSWC’s Audit Review Advisory Committee.
The project team determined that the function of auditing workers’ compensation providers could serve as a valuable means to:
- increase incentives for claims administrators to deliver benefits in a timely and accurate manner,
- identify and correct locations with poor claims administration,
- reduce the impact of poor performers on the delivery of benefits to workers, and
- assist stakeholders, where possible, to monitor system performance.
To accomplish these goals, the audit process requires mechanisms that:
- accurately measure the performance of claims administrators, and
- select audit subjects in a manner that it is fair and efficient, i.e.
1) Problems are highly likely to be identified.
2) Good performers are unlikely to be targeted.
3) Poor performers are targeted early on.
The audit function should also be carried out:
- at minimum cost to the taxpayer, and
- without undue burden upon the insurer, claims administrator, or employer.
Meetings with the Workers’ Compensation Community
The Audit Project research team met with representatives from the workers’ compensation community, including:
- Consultants from the Legislative Committees,
- DWC Administrative Director,
- Area Manager and Staff from the Division of Workers’ Compensation,
- DWC Audit Manager and selected Audit staff,
- Department of Insurance (CDI) Legal Counsel,
- Chief of the CDI Consumer Services Division,
- Representatives from the California Workers’ Compensation Institute,
- Representatives from the California Applicants’ Attorneys Association, and
- State Compensation Insurance Fund Claims/Rehabilitation manager.
The research questions that the project team employed as a guideline for the interviews are shown in Appendix E.
The research team also conducted an on-site review of claims handling practices and procedures at a major insurer in Southern California.
Survey of Audit Programs in Other States
Several states were contacted with requests for information regarding their workers’ compensation audit program, if any. Responses were received from Arizona, Colorado, Florida, Oregon, Texas, and Wisconsin. Appendix F contains a brief description of the workers’ compensation audit programs in those states.
The research team focused on the following areas:
- Review of Audit Unit documents and data
- Review of Department of Insurance documents and audit procedures
- Review of legal provisions and mandates
- Preliminary review of benefit notice provisions
- Review of audit programs in other states
- Review of insurer payment data to estimate the cost of a single rate of compensation
- Review of DWC Workers’ Compensation Information System (WCIS) regulations and DWC Audit Unit regulations, including revisions effective November 25, 1998.
Comments on the initial draft report
The project team issued an initial draft report in June 1998 for review and comment by the Commission and the Advisory Committee. The Advisory Committee was in general agreement on the initial draft report and its recommendations, but requested details and further clarification of the recommendations.
The Commission reviewed the initial draft and requested further clarification in several areas:
- Detailed description of the proposed revised workers’ compensation audit process;
- Assessment of the impact of establishing a single rate for all species of compensation and simplifying the calculation of the permanent disability benefit;
- Additional definition and discussion of the proposed penalty structure;
- Identification and description of the proposed key indicators.
This revised report includes the update and expansion of the proposed recommendations as requested by the Commission and the Advisory Committee.
We believe that an audit function is an important and necessary component of the California workers’ compensation system. If staffed appropriately and focused on critical areas, a workers’ compensation audit function will continue to be a useful tool to ensure prompt and accurate delivery of benefits to industrially-injured workers.
The research team found the staff of the Audit Unit to be very knowledgeable, dedicated, and highly professional in their approach to and completion of their duties within the current parameters of the audit function. Suggestions for changes in this report should not be construed as criticism of overall Audit Unit staff performance.
However, we have determined that improvements could and should be made to this vital program. The following are findings on which the Legislature, the Commission, the DWC, and the workers’ compensation community could base decisions to improve this function in the State of California.
Findings were noted in the following areas, each of which is discussed further:
- Scope of audit function
- Audit process
- Audit penalties
- System complexity
- System performance measures
- Audit function administration
- Observations by Audit Unit staff
- The current audit function concentrates excessive resources on detailed audits in relatively few locations.
- It takes several auditors in one location over a month to complete one audit.
- Most locations are rarely subject to audit.
- Of the 600 possible locations subject to audit, 39 were done in 1997 and an estimated 33 will be completed in 1998. At the current pace it would take 21 years for all locations to be randomly audited.
- The current audit function does not provide optimum capability to identify and improve poor claims handling. Only a few audits are targeted at the worst performers.
- Audits resources are focused on numerous minor violations and are not primarily directed at key events – those that cause the most impact on the injured worker.
- The current audit methodology is very cumbersome.
- The current audit procedures are time consuming, requiring DWC Audit Unit staff to spend on average approximately four hours per indemnity claim.
- Only the two most recent full calendar years of claims files are being reviewed during the current audits. The more severe claims that involve a long time to resolution -- and are likely to have higher indemnity and medical payments and more violations -- are not reviewed when mature.
- Claims administrators are subject to over one month disruption due to auditor’s presence in the office reviewing files.
Audit Subject Selection Process
The current process to select insurers for random and non-random audits is problematic. Appendix G includes further discussions and analyses of the current audit selection process.
- The random audit selection process is inequitable and does not result in proportional representations of the total population of claims or locations.
- Each location is given the same likelihood of being selected for a random audit. Consequently, claims at smaller locations of insurers with more decentralized administration are more likely to be audited.
- A self-administered self-insured employer with several hundred claims is just as likely to be audited as a large centralized insurer with 100,000 claims.
- The listing of potential audit locations from which random audits are selected may not be complete.
- There is only a small probability that any particular entity will be selected for audit in any year. At 1997 rates, the Audit Unit would randomly audit all locations once every 21 years. Some audit subjects can be selected multiple times.
- Few targeted audits are being performed. Between 1993 and 1997, 86% of all audits were random audits. The worst performers are not being targeted aggressively under this system.
- When targeting, the Audit Unit relies on complaints collected in a nonsystematic way. This leads to bias and less effective targeting.
Estimating system-wide performance based on the sample of audited locations is complicated by the changes, year to year, in the distribution of random and targeted audits. Since these have very different performance characteristics, the proportion of targeted and random audits affects the data published each year by the Audit Unit.
From random and targeted audits conducted in 1995, 1996, and 1997, the following categories of infractions were most often cited:
- Failure to timely provide proper and accurate benefit notices
- Late indemnity payments
- Failure to pay accrued and payable indemnity in undisputed claims
- Failure to timely comply with vocational rehabilitation notice requirements
- Failure to pay or object to medical or medical-legal bills within 60 days of receipt
Appendix H
contains a table showing the numbers and monetary fines of the five most common audit penalties cited in random and nonrandom audits in 1995, 1996, and 1997.- The current penalty structure concentrates small penalties on a large number of violations rather than large penalties on critical violations.
- The current penalty structure is insufficient to motivate improvement by the worst performers.
- The current penalty structure is unfair to smaller entities and provides minimal incentive to large entities.
- The current civil penalty investigation and assessment process is inefficient, ineffective, and absorbs excessive Audit Unit resources.
- Labor Code Section 129.5 is vague and needs further clarification.
The workers’ compensation benefit delivery process was made more complicated by the 1989 and 1993 reforms. These complexities may have implications for some of the violations cited in the DWC Audit Unit Annual Reports.
- The DWC Audit Unit Annual Report data on compensation due has been often cited for estimates of the amount of compensation due systemwide, and for trends in the rate of underpayment. However, the changing system complexities hinder the determination of trends in the level of unpaid compensation in the system, an area that has received particular attention from the Legislature.
- System complexities also affect the Benefit Notice Program and the consequent ability of claims administrators to communicate with workers and the ability of workers to understand the benefits they receive.
- An extensive and detailed discussion of the complexity of the benefit delivery process is included in Appendix I.
Determining ‘Compensation Due’
Difficulties in evaluating the amount of and trends in compensation due are exacerbated by
- definitions used by the Audit Unit to define compensation due,
- statutory changes in payment rates,
- complexities in benefit calculations, and
- the changing composition of the sample of audit subjects drawn by the DWC.
An analysis of the amounts of compensation due for 1997 as determined by the DWC Audit Unit is contained in Appendix J.
Definition of ‘Compensation Due’
The Audit Unit includes under "unpaid compensation" both
- compensation that would not have been paid except for the intervention of the Audit Unit, (e.g., unpaid Temporary Disability on a closed claim), and
- compensation that would have been paid, but was not paid at the time of the Audit.
In the latter category are PD payments that were begun on the date that the injured worker’s medical condition became permanent and stationary (P&S). But, if the claims examiner should have made payments retroactively to the date of the termination of TD benefits, then these payments are considered ‘unpaid’ rather than ‘late’.
Statutory changes in payment rates
Since 1991, several changes have been made in the maximum weekly rate of PPD payments and in the multiples of weeks of PPD received for each percent of disability. As a result, the range over which errors in the estimation of compensation payments can be made as a result of miscalculations in the average weekly earnings (AWE) at injury has increased. Also, the dollars of compensation that can be in dispute have also increased.
In 1991, the maximum weekly payment for PPD was $140; consequently workers earning more than $210/week met the maximum and additional calculations were unnecessary. For injuries on or after July 1, 1996, the PPD maximum ranged from $140 for disability ratings below 15% to $230 for those with ratings 70% and above. Careful recalculation of PD based on AWE is necessary for workers earning up to $345.
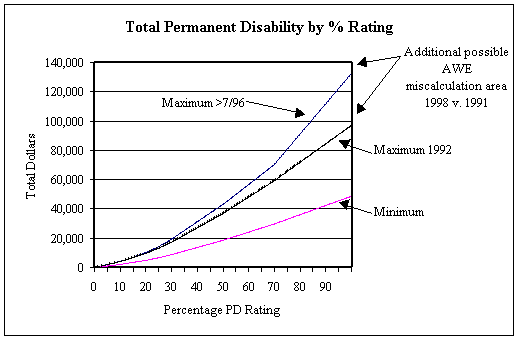
Claims benefit calculations are complicated and sometimes prone to error. First, permanent Disability benefits are calculated on a basis that requires adjustments for the number of weeks per rating point and the maximum weekly amount, as the rating estimate changes. Claims examiners are required to estimate the PD rating at the end of TTD which may be well in advance of the P&S report. A number of changes can be required in the rate as additional information on the workers condition becomes available.
Second, as complicated as these calculations are to the claims examiner, they are likely to be even more difficult for the injured worker to understand. The worker receives different weekly rates for TTD, PD and VRMA. In addition, the TD and the PD weekly rate could change several times over the life of the claim.
The benefit notice program is intended to be a key communication tool between the claims administrator and the injured worker, keeping the worker informed about important changes in the status of his or her claim.
However this review finds that:
- The Benefit Notice system is complex, cumbersome, and not currently designed to provide meaningful information to injured workers regarding benefit levels or to collect appropriate data to monitor prompt delivery of proper benefits.
- Current benefit notices are not readily comprehensible and result in confusion to injured workers and all parties. (For further information, please refer to the CHSWC report "Navigating the California Workers’ Compensation System: The Injured Worker Experience". This point was also brought up in testimony by an injured worker at the CHSWC public fact-finding hearing on anti-fraud activities.)
- "Failure to timely provide proper and accurate benefit notices" is the category that consistently received the most audit citations in the targeted and random audits of insurers, TPAs, and self-insured employers in 1995, 1996, and 1997.
- Industry complaints have been received regarding the following topics pertaining to the Benefit Notice Program:
- The number of violations indicates that the benefit notice program may be overly cumbersome, confusing, and difficult to administer.
- Key measures are needed upon which to compare performance.
- The current benefit notice program may be a poor tool for communicating with workers.
Fifty percent of Audit Unit penalties are for violations of Benefit Notice requirements. The Audit Unit cited 15% of files (1997) for violations defined as ‘unpaid compensation’. Both of these problems arise at least in part because of the complexity of Benefit Notice process and the complexity of compensation calculations.
- The current audit function does not measure system-wide performance.
- Unpaid compensation in the system may be substantial, but estimates based on Audit Unit data may be unreliable.
- Unpaid compensation, as defined by the Audit Unit, may lead to misinterpretation by the public, and consequently overestimation of the seriousness of the problem.
- The limitation to auditing only relatively young claims may result in underestimation of unpaid compensation.
- Audit results are hard for participants to interpret when evaluating various claims administrators.
See Appendix K for a detailed discussion of the evaluation of data and the goals of the Audit Unit.
A table summarizing the activities of the Audit Unit is displayed in Appendix L. An analysis of those data shows that:
- Audit Unit production has declined from (top year) 1995 to 1997:
- Total audits have declined 39% from a high of 64 to an all-time low of 39.
- Number of claims files reviewed declined 48% from 16,261 to 8,504.
- Audit Unit production has declined from 1996 to 1997:
- Total audits have declined 29% from 55 to 39.
- Number of claims files reviewed declined 32% from 12,436 to 8,504.
- Audit Unit investigations have declined by over 50% from (top year) 1995 to 1997.
- As shown in the next section, these workload declines cannot be attributed to a decrease in filled Audit Unit positions.
- Note that the estimated numbers of Audit Unit activities for 1998 are projected to be less than 1997.
As shown in the following chart, the DWC Audit Unit had 62 authorized positions in 1993. Despite the number of authorized positions, the Audit Unit has been staffed at a fairly consistent level of about 25 positions from 1993 to 1997. The number of authorized positions for the Audit Unit has consequently declined dramatically from 62 in 1993 to 26 in 1997.
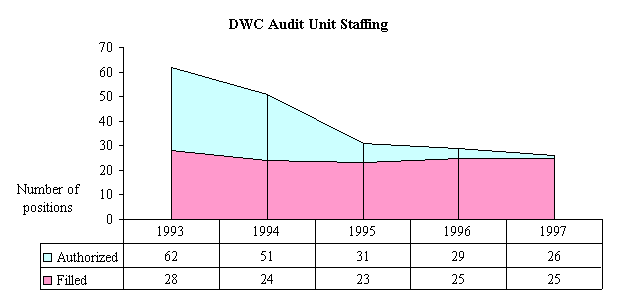
Audit Unit Statutory Requirements
- In the past year, approximately forty percent of the Audit Unit’s time was absorbed in conducting investigations to apply civil penalties of $100,000 under Labor Code Section 129.5(d). However, it is unclear that these fines are effective deterrents, or that this is an effective use of Audit Unit time. The Audit Unit has never invoked nor assessed this penalty.
- There is no clear understanding of what is required to establish a "civil penalty" under Labor Code Section 129.5(d). DWC auditors report that they currently have five auditors in Northern California and several in Southern California dedicated to one investigation. So far, this endeavor has taken two years and is continuing.
- The Department of Insurance (DOI) has advised that it has sufficient jurisdiction and authority under Insurance Code 790.035 to assess penalties on carriers. The DWC Audit Unit reports that, until May 1998, no such referrals had been made. The project team was informed that procedures are being set in place to coordinate efforts and referrals between DOI and DIR. Please refer to Appendix M for an analysis of the application of the Fair Claims Settlement Practices Act (Insurance Code Section 790.03(h)) to workers’ compensation.
- The DWC Administrative Director has the authority to audit and assess substantial penalties for failure to meet obligations under the Labor Code. Labor Code Sections 129 and 129.5 provide for the Insurance Commissioner to have authority over insurers regarding general business practices of unfair claims adjustment. Currently, there are no procedures in place for the DWC AD to make referrals to the Insurance Commissioner as contemplated by those sections.
Observations by Audit Unit Staff
- Follow-up audits have been conducted in a limited number of situations, but where they have been conducted, most locations have shown significant improvements. A few have not.
- There is a perception that claims examiners have varied levels of expertise and training.
- There appears to be an industry wide problem with vocational rehabilitation notice issuance.
- Obtaining the proper "date of knowledge" from employers is a problem for claims examiners and auditors.
- Medical providers use the Audit Unit to engage in "war with the claims administrator" by filing complaints on alleged down coding of bills. (The Audit Unit does not have authority to examine downcoding issues.) Investigations are being skewed by complaints reported by medical providers. As a consequence, targeting may be less efficient at identifying locations that fail to deliver accurate and timely benefits to injured workers.
- The audit unit staff believe the following to be the key indicators of performance:
- Unpaid compensation
- Failure to send notices
- Late benefit payments
- Unsupported denials
- "Duty to investigate" (Although not a direct indicator, it is perceived as an important factor throughout the audit.)
As a result of the Commission’s analyses and with the participation of the Advisory Committee, proposals are being made to address system shortcomings or failures. These include recommendations regarding the DWC Audit Function and other aspects of the California workers’ compensation system affecting benefit delivery.
Recommendations for the Audit function:
- Improve audit function administration and ensure sufficient staffing.
- Increase incentives for timely and accurate delivery of benefits.
- Improve targeting of poor performers.
- Revise audit process.
Recommendations for other aspects of the California workers’ compensation system affecting benefit delivery:
- Pay all benefits at a single weekly rate.
- Simplify the calculation of permanent disability.
- Improve the Benefit Notice program.
- Change mechanism for Commission funding.
Audit Function Recommendations
Improve audit function administration and ensure sufficient staffing
- Additional staff for the DWC Audit Unit are needed whether or not the current audit process continues or the recommended revisions are adopted. (Oregon has seventy auditors and a much smaller workers’ compensation program.) Some of the necessary personnel could possibly be redirected within the Division from areas where workload has dropped, such as the Rehabilitation Unit.
- The Audit Unit should employ a sufficient number of senior audit officers to ensure quality control and productivity.
- Performance monitoring of Audit Unit production should be addressed by the Division of Workers’ Compensation.
- The DWC needs to provide updated equipment, such as portable computers, to facilitate the audit process.
- There may be a conflict of interest with respect to the DWC Administrative Director conducting hearings on the possible assessment of the $100,000 penalty per Labor Code Section 129.5(d). The feasibility should be explored of modifying the Labor Code to permit such hearings to be conducted by another entity in DIR, such as the WCAB.
- The DWC Administrative Director should take more assertive action on identifying entities and assessing applicable $100,000 penalties per Labor Code Section 129.5(d). (Note: Most Audit Advisory Committee members were in accord that the DWC AD had "set the bar too high" to pursue the possible application of the $100,000 penalty.)
- The DWC Administrative Director should establish a system by which referrals are made to the Department of Insurance, pursuant to the provisions of Labor Code Section 129.5(d) and Insurance Code Section 790 et. seq.
Increase incentives for timely and accurate delivery of benefits
Current audit penalty structures impose disproportionate burdens on some claims locations, while providing little incentives to other locations.
Most CHSWC Audit Advisory Committee members were in accord that the penalty process should be changed in two ways:
- Eliminate penalties on good performers, and
- When applying penalties to poor performing locations, adjust penalties relative to the number of claims in the population of claims subject to audit.
Eliminating penalties on good performers will acknowledge good claims practices and help focus attention on the poorest performing locations. Adjusting penalties relative to the size of the claims location will improve the incentives associated with penalties while making the burden apply more equitably across big and small locations.
The project team also recommends improving the audit function’s effectiveness through increasing the use of audits that are targeted.
Penalty levels should be increased for key factors and reduced or eliminated for minor problems.
Improve targeting of poor performers
Current targeting is based on complaints filed with the Audit Unit. However, few complaints are collected and those collected are systematically biased. This means that targeting is unlikely to be fair or accurate. See Appendix N for a discussion on the current targeting process.
The Commission recommends increasing the identification and collection of complaints and to systematically collect complaints in a way that will improve the accurate identification of targeted audit locations.
Proposals include improving the detection and evaluation of complaints through I&A offices, development of a complaint evaluation capability within the Audit Unit, and increased emphasis on complaint referrals from Workers’ Compensation Judges and Rehabilitation Unit Counselors. More systematic collection of complaints from injured workers, through I&A, will reduce the time necessary to identify poor performers. Increasing reliance on WCJs and I&A Officers will reduce the current bias towards targeting based on medical provider complaints.
The DWC AD and other senior management need to place emphasis on complaint referrals as an important and critical component of a successful targeting process. Tracking of complaints by source should be re-instituted. In addition, mechanisms should be in place to refer complaints to the appropriate unit when resolution is possible and offices should be rewarded with recognition for consistent and accurate use of the referral process.
Complaint evaluation should be done by the Audit Unit. This could be done as it is currently by weighting the complaint by the source of referral. This is a de facto evaluation of the quality of the complaint. Secondarily, the Audit Unit could assess the value of the complaint based on experience. That is, the complaint may have no merit on its face, or the complainant may be well known for constant filings.
Given this additional evaluation of complaints, and assuming that complaint filings increase as attention of judges, rehabilitation consultants and I&A officers is focused on this area, the need for on site investigations of the complaint files to establish the validity of the complaint might be eliminated. This intermediate stage in the targeting process may be unnecessary.
In addition, the DWC should consider having complaints by injured workers with merit referred to I&A for follow-up. This would allow correction of the problem, something that is not currently within the scope of the Audit Unit function.
Complaints are currently compiled and assigned points by the Audit Unit based upon what type of entity (injured worker, medical provider, etc.) is making the referral. These are not investigated unless and until the pertinent location is selected for audit. Both validating the complaints and responding to the complainant were suggested as good public policy and practice.
Overview of Proposed Audit Process
Under current DWC audit procedures, locations are rarely subject to random audits and almost never subject to targeted audits. The Commission recommends the replacement of current audit procedures with one or all of the following:
- Simplified audit, focusing on key violations.
- Auditing of all locations on a five-year cycle.
- Electronic monitoring of key performance indicators where possible.
- Increased use of targeted audits to identify poor performers.
The results of the routine audits should be used to:
- Identify poor performers for an in-depth review.
- Verify data integrity.
- Benchmark performance on key indicators.
- Rank performance of adjusting locations.
Highlights of Proposed Changes
- Every location would be subject to a screening audit, called a Profile Audit Review (PAR), once every five years. The PAR is intended to identify the 5% to 10% ‘worst performers’.
- Those locations which pass the PAR would pay any compensation due but would not pay administrative penalties.
- Those locations that fail the PAR (the 5% to 10% ‘worst performers’) would undergo a rigorous audit, called the Full Compliance Audit (FCA).
- Those locations passing the FCA would pay compensation due and administrative penalties associated with unpaid or late paid compensation at the level of current administrative penalties.
- Those locations failing the FCA would pay compensation due and penalties according to the proposed FCA Penalty Schedule on all violations.
- Based upon complaints or other indications of inadequate performance, a location may be targeted for a PAR or FCA audit at any time.
- Each location doing workers’ compensation business in California would be routinely subject to a Profile Audit Review (PAR) once every five years by the Audit Unit of the Division of Workers’ Compensation.
- The DWC Claims Unit, which processes claims against the Uninsured Employers Fund, would also be routinely subject to a Profile Audit Review (PAR) once every five years.
- Audits would be conducted on a particular location, unless the DWC Audit Manager determines that a company-wide audit is more appropriate.
- Each location would undergo the initial screening audit, called the Profile Audit Review (PAR), designed to identify those locations with the ‘worst performance’.
- Casefiles would be selected for audit according to the PAR Selection Process.
- Whether or not a location passes the PAR audit would depend upon its performance with respect to the PAR Performance Standard.
- If a location passes the PAR audit
- No administrative penalties would be assessed. (For a discussion of this recommendation, see Appendix O)
- The location would be required to pay any compensation due, including self-imposed increases pursuant to Labor Code Section 4650(d).
- The location would not be subject to another audit for five years, unless it is targeted for audit based on target criteria.
- If a location fails the PAR audit
- The location would be required to pay any compensation due, including self-imposed increases pursuant to Labor Code Section 4650(d).
- The location would undergo a Full Compliance Audit (FCA).
- The Full Compliance Audit (FCA) is a comprehensive and detailed evaluation of a location’s performance.
- A location would undergo a FCA audit
- If the location fails a PAR audit, or
- If the location is targeted for a FCA audit.
- Casefiles would be selected for audit according to the FCA Selection Process.
- Whether or not a location passes the FCA audit would depend upon its performance with respect to the FCA Performance Standards.
- If a location passes the FCA audit
- The location would be required to pay any compensation due, including self-imposed increases pursuant to Labor Code Section 4650(d).
- The location would pay administrative penalties associated with unpaid or late paid compensation. These administrative penalties are at the level of the current administrative penalties.
- The location would not be subject to another audit for five years, unless it is targeted for audit based on target criteria.
- If a location fails the FCA audit
- The location would be required to pay any compensation due, including self-imposed increases pursuant to Labor Code Section 4650(d).
- The location would be required to pay penalties according to a FCA Failure Penalty Schedule adjusted to the size of the audit location.
- The location would undergo a follow-up Full Compliance Audit (FCA) within two years.
- Failure to pass two consecutive FCAs would constitute prima facie evidence of civil violations as described in Labor Code Section 129.5(d).
- A location could be targeted for audit at any time, whether or not it recently had been audited.
- The target audit criteria would be used to identify locations for audit.
- Based on target audit criteria factors such as complaints, targeted locations would undergo a PAR.
- Under extraordinary circumstances as defined by target audit criteria, targeted locations would be subject to undergo a FCA audit without first having a PAR audit.
- Whether or not a location passes a targeted audit would depend upon its performance with respect to the PAR Performance Standard or to the FCA Performance Standard, as appropriate.
- Targeted locations failing the PAR audit and/or the FCA audit would be subject to the same consequences as locations otherwise undergoing PAR and/or FCA audits.
Audit Sample Selection Process
- 25% from the most recent year prior to the audit year;
- 50% from the year two years prior to the audit year; and
- 25% from open claims from years three and four years prior to the audit year.
- Sample sizes would reflect those currently established in regulations
- Medical-only files will be reviewed
- Files would be sampled in the following proportions:
- 25% from the most recent year prior to the audit year;
- 50% from the year two years prior to the audit year; and
- 25% from open claims from years three and four years prior to the audit year.
- Audits would be on the entire sample and not abbreviated based on results of the first half of the audit.
- Complaint files would be included in the FCA audit.
- The PAR is intended to identify the worst performers so that they may be audited in detail through the FCA.
- To pass a PAR, the location would have to meet or exceed the PAR Performance Standard. See Appendix P for a discussion of the PAR and FCA performance standards.
- The PAR Performance Standard is a composite score, based upon the PAR Key Indicators.
- The PAR Key Indicators are as follows:
- The denial of a claim is appropriately supported by a medical, factual or legal basis.
- The initial notice and the first Temporary Disability payment are timely and accurate.
- All indemnity (TD, PD, and VRMA) due has been paid.
- First payments of PD, VRMA and death benefits have been timely delivered.
- Compliance with AME/QME notice requirements upon a P&S designation has been achieved.
- Vocational rehabilitation benefits have been appropriately offered.
- The PAR Performance Standard considers all of the six PAR key indicators and weights Key Indicators #1 and #3 more heavily than the others.
- Note that the PAR Performance Standard would be evaluated each year.
- The FCA is intended to determine where the ‘worst performers’ are failing in the timely delivery of workers’ compensation benefits.
- To pass a FCA, the location would need to meet or exceed the FCA Performance Standard.
- The FCA Performance Standard mirrors the PAR Performance Standard except that the number of criteria involved in the composite score is expanded to include all administrative violations and not just the six Key Indicators. See Appendix P for a discussion of the PAR and FCA performance standards.
Passing/Failing a Targeted Audit
- A Targeted Audit is intended to determine if a particular location is failing in the timely delivery of workers’ compensation benefits.
- Whether or not a location passes a targeted audit would depend upon its performance with respect to the PAR Standard or to the FCA Standard, as appropriate.
- Targeted locations failing the PAR audit and/or the FCA audit would be subject to the same consequences as locations otherwise undergoing PAR and/or FCA audits.
The Commission Research Team found that the current audit penalty structure offered insufficient incentives for good performance and was biased in its application. The Project Research Team recommends a penalty structure that would:
- Eliminate penalties for entities that meet or beat threshold levels of violations.
- Adjust penalty levels relative to the size of the entity or location.
These changes are meant to:
- Make the audit process more efficient;
- Increase incentives for poor performers to improve claims administration; and
- Eliminate the unequal application of penalties across entities of different sizes and different levels of decentralization.
If a location fails the FCA, the location would be subject to the following administrative penalties, based on the size of the location and the size of the sample selected for the auditing process.
Table of Administrative Penalties

If a location passes at the FCA level, administrative penalties for unpaid or late paid compensation would be paid at the minimum level (Rank 1).
A discussion of the development of the proposed penalty structure is contained in Appendix Q.
A location would be targeted for a PAR audit in response to
- complaints received about the location’s performance,
- concerns expressed by the workers’ compensation community, or
- other indications.
A location could be targeted for a FCA audit by the DWC Audit Manager in response to
- extraordinary circumstances, or
- other serious indications.
Ranking of Locations According to Performance
- Locations would be ranked according to their performance measured by the DWC Audit PAR Performance Standard.
- Those Location Performance Rankings would be published and made available to the workers’ compensation community and to the public on request.
Other Workers’ Compensation System Recommendations
Although not directly within the purview of the audit function, the following recommendations are made to address current systemic problems within the workers’ compensation system affecting benefit delivery.
Pay all benefits at a single weekly rate
The industrially injured worker receives payment at different weekly rates for the various types of workers’ compensation benefits: Temporary Disability (TTD), Permanent Disability (PD), and the Vocational Rehabilitation Maintenance Allowance (VRMA). Both the TD and the PD weekly rate can change several times over the life of the claim.
The Audit Advisory Committee and the Commission Research Team suggest that an injured worker should receive payment for all types of indemnity at a single weekly rate. Under this proposal all benefits would be paid at the TTD rate regardless of the species of benefit. This will not change the total amount of benefits, only the rate at which they are paid out.
- For PPD benefits this is straightforward and is described in detail in Appendix R.
- For VRMA, the payments may exhaust the resources under the $16,000 cap more quickly. This will result in shorter plan duration or as recommended by the Audit Advisory Committee, the worker should be allowed to restore the ‘cap’ amount with permanent disability advances.
Changing the rate of payment, even if the total amount remains the same, has an implication for cash flow and interest earnings on reserves for insurers and self-insured employers. Since interest earnings are an important source of income for insurers and employers, a Commission member asked the research team to estimate the impact of this change. The Commission Research Team undertook this evaluation using a transaction dataset supplied by the California Workers’ Compensation Institute (CWCI). The Research Team determined that the impact would reduce insurer/employer earnings from interest income by an amount equal to between 0.2% and 0.4% of all benefit payments. These findings are detailed in Appendix R.
Simplify Permanent Disability Calculations
Calculating Permanent Disability benefits is complex for the claims administrator and confusing for the worker. In part this is because the weekly payment amount factors in a changing multiplier of weeks of payment as the seriousness of the disability increases, and a changing maximum rate as the seriousness of the disability increases. The logic for using changes on both of these dimensions is hard to understand. It is especially difficult to understand why the maximum is raised in a stepwise fashion as the disability level increases.
A simpler and fairer method would be to increase the ‘weeks’ multiplier more steeply and keep the maximums at the same level for all disability ratings. Besides being clearer, it would eliminate the need for claims examiners to re-compute the PPD rate based on average weekly earnings as the disability levels changed. This should also reduce the confusion of injured workers concerning their benefit calculation.
Note, however, that simplifying the calculation of the amount of PPD due by eliminating the stepped maximums in the weekly rate, while considered desirable by the Advisory Committee, will result in substantial changes in the level of compensation paid by employers or the distribution of compensation among different groups of workers. Therefore, the project team believes that this recommendation is more appropriately handled by the Commission’s PD Policy Advisory Committee in conjunction with CHSWC’s continuing overall evaluation of the Permanent Disability process.
Improve Benefit Notice Program
An automated, simplified benefit notice system with initial key indicators should be developed and implemented as a priority. This information is to be submitted electronically to the State of California. Those carriers who do not submit electronic versions of benefit notices may be selected for targeted or random audit on an ad hoc basis.
A committee should be established to review and make recommendations on streamlining the Benefit Notice process, reducing requirements, and ensuring that notices accurately and effectively communicate with injured workers in a format and language that is comprehensible. Particular attention should be focused on the requirements for notification of potential eligibility for vocational rehabilitation. These notices are the most commonly cited for violations and affect the most seriously injured workers.
The Commission has contracted with the Labor Occupational Health Program to assess the needs and explore methods for improving benefit notices to injured workers. The goals of this project are as follows:
- Identify the most significant problems with notices, from the injured workers’ perspective, that contribute to problems with claims.
- Develop practical criteria for improving, from the injured workers’ perspective, the notices that are currently required by the California Labor Code and the California Code of Regulations.
- Identify the statutory and regulatory requirements that cause the greatest problems with notices, from the injured workers’ perspective.
- Identify further, practical steps that the Commission might take to examine and address the statutory and regulatory requirements governing the content, volume, style of language, and timing of notices.
This project is expected to continue through 1999.
Change Mechanism for Commission Funding
In order to avoid the appearance of a conflict of interest, funding for CHSWC should not be totally dependent on the amount of the audit penalties collected by the DWC Audit Unit. Currently, audit collections are deposited into the Workplace Health and Safety Revolving Fund and the Commission’s budget is appropriated out of that fund. If audit collections are not sufficient to meet the needs of the Commission, there is currently no recourse.
The Commission proposes that audit collections be deposited into the state’s Workers' Compensation Administration Revolving Fund (see Labor Code Section 62.5) or into the State General Fund. An adequate amount for the Commission’s budget could then be appropriated from the state’s Workers' Compensation Administration Revolving Fund or from the State General Fund. If allocated from the state’s Workers' Compensation Administration Revolving Fund, the Commission’s budget would be included in the 80/20 funding ratio for workers’ compensation programs.
Implementing the New Audit System
- Revise Labor Code (See Appendix S for proposed changes.)
- Revise regulations
- Develop and distribute informational materials
- Provide training and information for insurers, self-insured self-administered employers and third-party administrators
- Training sessions- San Diego, Los Angeles, San Francisco, Sacramento
- Training packet
- Information on web site
- Hire and train additional staff for audit function
- Six month transition period for implementation
- Ensure that the DWC Workers’ Compensation Information System (WCIS) captures the essential data elements for the Audit Key Indicators.
Staffing Required for Revised Audit Process
The following table shows estimates of the full-time equivalent (FTE) requirements to conduct a simplified PAR audit of all claims adjusting locations on a 5-year cycle. These simplified PAR audits are intended to review files more quickly by focusing only on several key violations. Only if a location failed the simplified PAR audit, based on performance measures jointly developed by the DWC and the Commission, would a location be subject to a full FCA audit based on all violations. Locations would still be subject to the full FCA audit if targeted for audit based on complaints or previous audit performance.
Profile Audit Reviews (PAR) |
Full Compliance Audits (FCA) |
|
| Number of locations | 600 |
|
| Locations audited/year | 120 |
32 |
| Average files audited per location | 150 |
150 |
| Total files audited/year | 18,000 |
4,800 |
| Average hours/file | 1 hour |
3 hours |
| Total audit hours | 18,000 |
14,400 |
| Ratio of total hours/audit hours | 1.7 |
1.7 |
| Total staff time | 30,600 hours |
24,480 hours |
| Number of positions required | 17.2 |
13.8 |
These estimates will be low to the extent that 1 hour/file underestimates the time required to conduct a simplified audit on selected files based on an agreed set of key performance measures. If we wished to audit all locations using current procedures, these estimates should be multiplied by four.
These estimates will be high to the extent that currently proposed regulations to reduce the number of files audited at a given location reduce the average number of files audited per location. These reductions are based on the first files audited at a location meeting certain performance statistics.
If the concept of auditing all locations is not adopted, then changes should be made to the random sampling methodology to stratify locations by the number of claims reported for that location. This would increase the focus on claims locations that handle most injured workers’ claims.
The Commission on Health and Safety and Workers' Compensation would like to thank the following for their assistance in this study:
- The CHSWC Audit Study Advisory Committee;
- The Division of Workers Compensation Audit Unit and manager, Mark Johnson;
- The Department of Insurance;
- The California Workers' Compensation Institute for use of their CMOS claims data and for their feedback;
- The State Compensation Insurance Fund for their technical expertise and feedback;
- The California Applicants' Attorneys Association and their consultant Mark Gerlach for their analysis and feedback;
- The American Insurance Association for their feedback;
- Georgia Pacific Corporation for their feedback;
- Republic Indemnity for allowing research staff to observe their claims operations.
The following staff members made significant contributions to this report:
Christine Baker, CHSWC Executive Officer
C. L. Swezey, Esq., CHSWC Legal Consultant
Frank Neuhauser, University of California, Berkeley
Kirsten Str�mberg, CHSWC staff
Marie W. Wardell, Consultant.
California Labor Code Sections 129 and 129.5
Section 129 - Audits
(a) To make certain that injured workers, and their dependents in the event of their death, receive promptly and accurately the full measure of compensation to which they are entitled, the administrative director shall audit insurers, self-insured employers, and third-party administrators to determine if they have met their obligations under this code. At least half of the audit subjects shall be selected at random, and the remaining subjects shall be selected pursuant to subdivision (b). The results of audits of insurers shall be provided to the Insurance Commissioner and the results of audits of self-insured employers and third-party administrators shall be provided to the Director of Industrial Relations. Nothing in this section shall restrict the authority of the Director of Industrial Relations or the Insurance Commissioners to audit their licensees.
(b) The administrative director shall establish priorities for audits based on information obtained from the Benefit Notice program established under Section 138.4, through information and assistance services and other factual information that indicates an insurer, self-insured employer, or third-party administrator is failing to meet its obligations under this division or Division 4 (commencing with Section 3200) or the regulations of the administrative director.
- If, as a result of an audit, the administrative director determines that any compensation, interest, or penalty is due and unpaid to an employee or dependent, the administrative director shall issue and cause to be served upon the insurer, self-insured employer, or third-party administrator a notice of assessment detailing the amounts due and unpaid in each case, and shall order the amounts paid to the person entitled thereto. The notice of assessment shall be served personally or by registered mail in accordance with subdivision (c) of Section 11505 of the Government Code. A copy of the notice of assessment shall also be sent to the affected employee or dependent.
If the amounts are not paid within 30 days after service of a notice of assessment, the employer shall also be liable for reasonable attorney's fees necessarily incurred by the employee or dependent to obtain amounts due. The administrative director shall advise each employee or dependent still owed compensation after this 30-day period of his or her rights with respect to the commencement of proceedings to collect the compensation owed. Amounts unpaid because the person entitled thereto cannot be located shall be paid to the Workplace Health and Safety Revolving Fund. The Director of Industrial Relations shall promulgate rules and regulations establishing standards and procedures for the payment of compensation from moneys deposited into the Workplace Health and Safety Revolving Fund whenever the person entitled thereto applies for compensation.
(d) A determination by the administrative director that an amount is or is not due to an employee or dependent shall not in any manner limit the jurisdiction or authority of the appeals board to determine the issue.
(e) Annually, commencing on April 1, 1991, the administrative director shall publish a report detailing the results of audits conducted pursuant to this section during the preceding calendar year. The report shall include the name of each insurer, self-insured employer, and third-party administrator audited during that period. For each insurer, self-insured employer, and third-party administrator audited the report shall specify the total number of files audited, the number of violations found by type and amount of compensation, interest and penalties payable, and the amount collected for each violation.
These reports shall not identify the particular claim file which resulted in a particular violation or penalty. Except as required by this subdivision or other provisions of law, the contents of individual claim files and auditor's working papers shall be confidential. Disclosure of claim information to the administrative director pursuant to an audit shall not waive provisions of the Evidence Code relating to privilege.
Section 129.5 - Administrative and Civil Penalties; schedule of violations
(a) The administrative director shall assess an administrative penalty against an insurer, self-insured employer, or third-party administrator for any of the following:
(1) Failure to comply with the notice of assessment issued pursuant to subdivision (c) of Section 129 within 15 days of receipt.
(2) Failure to pay when due the undisputed portion of an indemnity payment, the reasonable cost of medical treatment of an injured worker, or a charge or cost of implementing an approved vocational rehabilitation plan.
(3) Failure to comply with any rule or regulation of the administrative director.
(b) The administrative director shall promulgate regulations establishing a schedule of violations and the amount of the administrative penalty to be imposed for each type of violation. The schedule shall provide for imposition of a penalty of up to one hundred dollars ($100) for each violation of the least serious type and for imposition of penalties in progressively higher amounts for more serious types of violations, with the penalty for the most serious types of violations to be set at up to five thousand dollars ($5,000) per violation. The administrative director is authorized to impose penalties pursuant to rules and regulations which give due consideration to the appropriateness of the penalty with respect to the following factors:
(1) The gravity of the violation.
(2) The good faith of the insurer, self-insured employer, or third-party administrator.
(3) The history of previous violations, if any.
- The frequency of the violations.
(c) The notice of penalty assessment shall be served personally or by registered mail in accordance with subdivision (c) of Section 11505 of the Government Code. The notice shall be in writing and shall describe the nature of the violation, including reference to the statutory provision or rule or regulation alleged to have been violated. The notice shall become final and the assessment shall be paid unless contested within 15 days of receipt by the insurer, self-insured employer, or third-party administrator.
(d) In addition to the penalty assessment permitted by subdivision (a), the administrative director may assess a civil penalty, not to exceed one hundred thousand dollars ($100,000), upon finding, after hearing, that an employer, insurer, or third-party administrator for an employer has knowingly committed and has performed with a frequency as to indicate a general business practice any of the following:
(1) Induced employees to accept less than compensation due, or made it necessary for employees to resort to proceedings against the employer to secure compensation due.
(2) Refused to comply with known and legally indisputable compensation obligations.
(3) Discharged or administered compensation obligations in a dishonest manner.
- Discharged or administered compensation obligations in a manner as to cause injury to the public or those dealing with the employer or insurer.
Upon a second or subsequent finding, the administrative director shall refer the matter to the Insurance Commissioner or Director of Industrial Relations and request that a hearing be conducted to determine whether the certificate of authority, certificate of consent to self-insure, or certificate of consent to administer claims of self-insured employer, as the case may be, should be revoked.
(e) An insurer, self-insured employer, or third-party administrator may file a written request for a conference with the administrative director within seven days after receipt of the notice of penalty assessment issued pursuant to subdivision (a) or (d). Within 15 days of the conference, the administrative director shall issue a notice of findings and serve it upon the contesting party by registered or certified mail. Any amount found due by the administrative director shall become due and payable 30 days after receipt of the notice of findings. The 30-day period shall be tolled during any appeal. A writ of mandate may be taken from the findings to the appropriate superior court upon the execution by the contesting party of a bond to the state in the principal sum that is double the amount found due and ordered by the administrative director, on the condition that the contesting party shall pay any judgment and costs rendered against it for the amount.
(f) Nothing in this section shall create nor eliminate a civil cause of action for the employee and his or her dependents.
- All moneys collected under this section shall be deposited in the State Treasury and credited to the Workplace Health and Safety Revolving Fund.
INSURANCE CODE SECTION 790-790.10
790. The purpose of this article is to regulate trade practices in the business of insurance in accordance with the intent of Congress as expressed in the Act of Congress of March 9, 1945 (Public Law 15, Seventy-ninth Congress), by defining, or providing for the determination of, all such practices in this State which constitute unfair methods of competition or unfair or deceptive acts or practices and by prohibiting the trade practices so defined or determined.
790.01. This article applies to reciprocal and interinsurance exchanges, Lloyds insurers, fraternal benefit societies, fraternal fire insurers, grants and annuities societies, insurers holding certificates of exemptions, motor clubs, nonprofit hospital associations, life agents, broker-agents, surplus line brokers and special lines surplus line brokers as well as all other persons engaged in the business of insurance.
790.02. No person shall engage in this State in any trade practice which is defined in this article as, or determined pursuant to this article to be, an unfair method of competition or an unfair or deceptive act or practice in the business of insurance.
790.03. The following are hereby defined as unfair methods of competition and unfair and deceptive acts or practices in the business of insurance.
(a) Making, issuing, circulating, or causing to be made, issued or circulated, any estimate, illustration, circular or statement misrepresenting the terms of any policy issued or to be issued or the benefits or advantages promised thereby or the dividends or share of the surplus to be received thereon, or making any false or misleading statement as to the dividends or share of surplus previously paid on similar policies, or making any misleading representation or any misrepresentation as to the financial condition of any insurer, or as to the legal reserve system upon which any life insurer operates, or using any name or title of any policy or class of policies misrepresenting the true nature thereof, or making any misrepresentation to any policyholder insured in any company for the purpose of inducing or tending to induce such policyholder to lapse, forfeit, or surrender his or her insurance.
(b) Making or disseminating or causing to be made or disseminated before the public in this state, in any newspaper or other publication, or any advertising device, or by public outcry or proclamation, or in any other manner or means whatsoever, any statement containing any assertion, representation or statement with respect to the business of insurance or with respect to any person in the conduct of his or her insurance business, which is untrue, deceptive, or misleading, and which is known, or which by the exercise of reasonable care should be known, to be untrue, deceptive, or misleading.
(c) Entering into any agreement to commit, or by any concerted action committing, any act of boycott, coercion or intimidation resulting in or tending to result in unreasonable restraint of, or monopoly in, the business of insurance.
(d) Filing with any supervisory or other public official, or making, publishing, disseminating, circulating, or delivering to any person, or placing before the public, or causing directly or indirectly, to be made, published, disseminated, circulated, delivered to any person, or placed before the public any false statement of financial condition of an insurer with intent to deceive.
(e) Making any false entry in any book, report, or statement of any insurer with intent to deceive any agent or examiner lawfully appointed to examine into its condition or into any of its affairs, or any public official to whom the insurer is required by law to report, or who has authority by law to examine into its condition or into any of its affairs, or, with like intent, willfully omitting to make a true entry of any material fact pertaining to the business of the insurer in any book, report, or statement of the insurer.
(f) Making or permitting any unfair discrimination between individuals of the same class and equal expectation of life in the rates charged for any contract of life insurance or of life annuity or in the dividends or other benefits payable thereon, or in any other of the terms and conditions of the contract.
This subdivision shall be interpreted, for any contract of ordinary life insurance or individual life annuity applied for and issued on or after January 1, 1981, to require differentials based upon the sex of the individual insured or annuitant in the rates or dividends or benefits, or any combination thereof. This requirement is satisfied if those differentials are substantially supported by valid pertinent data segregated by sex, including, but not necessarily limited to, mortality data segregated by sex.
However, for any contract of ordinary life insurance or individual life annuity applied for and issued on or after January 1, 1981, but before the compliance date, in lieu of those differentials based on data segregated by sex, rates, or dividends or benefits, or any combination thereof, for ordinary life insurance or individual life annuity on a female life may be calculated as follows: (a) according to an age not less than three years nor more than six years younger than the actual age of the female insured or female annuitant, in the case of a contract of ordinary life insurance with a face value greater than five thousand dollars ($5,000) or a contract of individual life annuity; and (b) according to an age not more than six years younger than the actual age of the female insured, in the case of a contract of ordinary life insurance with a face value of five thousand dollars ($5,000) or less. "Compliance date" as used in this paragraph shall mean the date or dates established as the operative date or dates by future amendments to this code directing and authorizing life insurers to use a mortality table containing mortality data segregated by sex for the calculation of adjusted premiums and present values for nonforfeiture benefits and valuation reserves as specified in Sections 10163.5 and 10489.2 or successor sections.
Notwithstanding the provisions of this subdivision, sex based differentials in rates or dividends or benefits, or any combination thereof, shall not be required for (1) any contract of life insurance or life annuity issued pursuant to arrangements which may be considered terms, conditions, or privileges of employment as these terms are used in Title VII of the Civil Rights Act of 1964 (Public Law 88-352), as amended, and (2) tax sheltered annuities for employees of public schools or of tax exempt organizations described in Section 501(c)(3) of the Internal Revenue Code.
(g) Making or disseminating, or causing to be made or disseminated, before the public in this state, in any newspaper or other publication, or any other advertising device, or by public outcry or proclamation, or in any other manner or means whatever, whether directly or by implication, any statement that a named insurer, or named insurers, are members of the California Insurance Guarantee Association, or insured against insolvency as defined in Section 119.5. This subdivision shall not be interpreted to prohibit any activity of the California Insurance Guarantee Association or the commissioner authorized, directly or by implication, by Article 14.2 (commencing with Section 1063).
(h) Knowingly committing or performing with such frequency as to indicate a general business practice any of the following unfair claims settlement practices:
(1) Misrepresenting to claimants pertinent facts or insurance policy provisions relating to any coverages at issue.
(2) Failing to acknowledge and act reasonably promptly upon communications with respect to claims arising under insurance policies.
(3) Failing to adopt and implement reasonable standards for the prompt investigation and processing of claims arising under insurance policies.
(4) Failing to affirm or deny coverage of claims within a reasonable time after proof of loss requirements have been completed and submitted by the insured.
(5) Not attempting in good faith to effectuate prompt, fair, and equitable settlements of claims in which liability has become reasonably clear.
(6) Compelling insureds to institute litigation to recover amounts due under an insurance policy by offering substantially less than the amounts ultimately recovered in actions brought by the insureds, when the insureds have made claims for amounts reasonably similar to the amounts ultimately recovered.
(7) Attempting to settle a claim by an insured for less than the amount to which a reasonable man would have believed he was entitled by reference to written or printed advertising material accompanying or made part of an application.
(8) Attempting to settle claims on the basis of an application which was altered without notice to, or knowledge or consent of, the insured, his or her representative, agent, or broker.
(9) Failing, after payment of a claim, to inform insureds or beneficiaries, upon request by them, of the coverage under which payment has been made.
(10) Making known to insureds or claimants a practice of the insurer of appealing from arbitration awards in favor of insureds or claimants for the purpose of compelling them to accept settlements or compromises less than the amount awarded in arbitration.
(11) Delaying the investigation or payment of claims by requiring an insured, claimant, or the physician of either, to submit a preliminary claim report, and then requiring the subsequent submission of formal proof of loss forms, both of which submissions contain substantially the same information.
(12) Failing to settle claims promptly, where liability has become apparent, under one portion of the insurance policy coverage in order to influence settlements under other portions of the insurance policy coverage.
(13) Failing to provide promptly a reasonable explanation of the basis relied on in the insurance policy, in relation to the facts or applicable law, for the denial of a claim or for the offer of a compromise settlement.
(14) Directly advising a claimant not to obtain the services of an attorney.
(15) Misleading a claimant as to the applicable statute of limitations.
(16) Delaying the payment or provision of hospital, medical, or surgical benefits for services provided with respect to acquired immune deficiency syndrome or AIDS-related complex for more than 60 days after the insurer has received a claim for those benefits, where the delay in claim payment is for the purpose of investigating whether the condition preexisted the coverage. However, this 60-day period shall not include any time during which the insurer is awaiting a response for relevant medical information from a health care provider.
790.034. Regulations adopted by the commissioner pursuant to this article which relate to the settlement of claims shall take into consideration settlement practices by classes of insurers.
790.035. (a) Any person who engages in any unfair method of competition or any unfair or deceptive act or practice defined in Section 790.03 is liable to the state for a civil penalty to be fixed by the commissioner, not to exceed five thousand dollars ($5,000) for each act, or, if the act or practice was willful, a civil penalty not to exceed ten thousand dollars ($10,000) for each act. The commissioner shall have the discretion to establish what constitutes an act. However, when the issuance, amendment, or servicing of a policy or endorsement is inadvertent, all of those acts shall be a single act for the purpose of this section.
(b) The penalty imposed by this section shall be imposed by and determined by the commissioner as provided by Section 790.05. The penalty imposed by this section is appealable by means of any remedy provided by Section 12940 or by Chapter 5 (commencing with Section 11500) of Part 1 of Division 3 of Title 2 of the Government Code.
790.036. (a) It is an unfair and deceptive act or practice in the business of insurance for an insurer to advertise insurance that it will not sell.
(b) Nothing in this section shall be construed to prohibit any insurer from advertising insurance products for which it is licensed to sell in this state where the product is not available for sale so long as the unavailability is disclosed in the advertisement.
(c) A violation of this section is subject to the sanctions provided for by this article.
(d) An intentional violation of this section is a misdemeanor punishable by a fine not exceeding ten thousand dollars ($10,000).
(e) This section does not apply to any insurer that refuses to sell a policy of insurance on the basis of its underwriting guidelines.
(f) This section does not apply to advertisements by an insurer where the advertisements are broadcast and originate from outside this state. As used in this subdivision, "broadcast" includes electronic media, television, and radio. As used in this subdivision, "originate from outside this state" includes cable transmittal of programs broadcast by stations located outside California.
790.04. The commissioner shall have power to examine and investigate into the affairs of every person engaged in the business of insurance in the State in order to determine whether such person has been or is engaged in any unfair method of competition or in any unfair or deceptive act or practice prohibited by Section 790.03 or determined pursuant to this article to be an unfair method of competition or an unfair or deceptive practice in the business of insurance. Such investigation may be conducted pursuant to Article 2 (commencing at Section 11180) of Chapter 2, Part 1, Division 3, Title 2 of the Government Code.
790.05. Whenever the commissioner shall have reason to believe that such person has been engaged or is engaging in this state in any unfair method of competition or any unfair or deceptive act or practice defined in Section 790.03, and that a proceeding by the commissioner in respect thereto would be to the interest of the public, he or she shall issue and serve upon that person an order to show cause containing a statement of the charges in that respect, a statement of that person's potential liability under Section 790.035, and a notice of a hearing thereon to be held at a time and place fixed therein, which shall not be less than 30 days after the service thereof, for the purpose of determining whether the commissioner should issue an order to that person to, pay the penalty imposed by Section 790.035, and to cease and desist those methods, acts, or practices or any of them.
If the charges or any of them are found to be justified the commissioner shall issue and cause to be served upon that person an order requiring that person to pay the penalty imposed by Section 790.035 and to cease and desist from engaging in those methods, acts, or practices found to be unfair or deceptive.
The hearing shall be conducted in accordance with the Administrative Procedure Act, Chapter 5 (commencing at Section 11500) of Part 1 of Division 3 of Title 2 of the Government Code, and the commissioner shall have all the powers granted therein.
The person shall be entitled to have the proceedings and the order reviewed by means of any remedy provided by Section 12940 of this code or by the Administrative Procedure Act.
790.06. (a) Whenever the commissioner shall have reason to believe that any person engaged in the business of insurance is engaging in this State in any method of competition or in any act or practice in the conduct of such business which is not defined in Section 790.03 and that such method is unfair or that such act or practice is unfair or deceptive and that a proceeding by him in respect thereto would be in the interest of the public, he may issue and serve upon such person an order to show cause containing a statement of the methods, acts or practices alleged to be unfair or deceptive and a notice of hearing thereon to be held at a time and place fixed therein, which shall not be less than 30 days after the service thereof, for the purpose of determining whether the alleged methods, acts or practices or any of them should be declared to be unfair or deceptive within the meaning of this article.
The hearings provided by this section shall be conducted in accordance with the Administrative Procedure Act, Chapter 5 (commencing at Section 11500) of Part 1, Division 3, Title 2 of the Government Code, and the commissioner shall have all the powers granted therein. If the alleged methods, acts, or practices or any of them are found to be unfair or deceptive within the meaning of this article the commissioner shall issue and service upon said person his written report so declaring.
(b) If such report charges a violation of this article and if such method of competition, act or practice has not been discontinued, the commissioner may, through the Attorney General of this State, at any time after 30 days after the service of such report cause a petition to be filed in the superior court of this State within the county wherein the person resides or has his principal place of business, to enjoin and restrain such person from engaging in such method, act or practice. The court shall have jurisdiction of the proceeding and shall have power to make and enter appropriate orders in connection therewith and to issue such writs as are ancillary to its jurisdiction or are necessary in its judgment to prevent injury to the public pendente lite.
(c) A transcript of the proceedings before the commissioner, including all evidence taken and the report and findings shall be filed with such petition. If either party shall apply to the court for leave to adduce additional evidence and shall show, to the satisfaction of the court, that such additional evidence is material and there were reasonable grounds for the failure to adduce such evidence in the proceeding before the commissioner, the court may order such additional evidence to be taken before the commissioner and to be adduced upon the hearing in such manner and upon such terms and conditions as to the court may seem proper. The commissioner may modify his findings of fact or make new findings by reason of the additional evidence so taken, and he shall file such modified or new findings with the return of such additional evidence.
(d) If the court finds that the method of competition complained of is unfair or that the act or practice complained of is unfair or deceptive, that the proceeding by the commissioner with respect thereto is to the interest of the public and that the findings of the commissioner are supported by the weight of the evidence, it shall issue its order enjoining and restraining the continuance of such method of competition, act or practice.
790.07. Whenever the commissioner shall have reason to believe that any person has violated a cease and desist order issued pursuant to Section 790.05 or a court order issued pursuant to Section 790.06, after the order has become final, and while the order is still in effect, the commissioner may, after a hearing at which it is determined that the violation was committed, order that person to forfeit and pay to the State of California a sum not to exceed five thousand dollars ($5,000) plus any penalty due under Section 790.05, which may be recovered in a civil action, except that, if the violation is found to be willful, the amount of the penalty may be a sum not to exceed fifty-five thousand dollars ($55,000) plus the penalty due under Section 790.05.
For the purposes of this section, the failure to pay any penalty imposed pursuant to Section 790.035 which has become final shall constitute a violation of the cease and desist order.
For any subsequent violation of the cease and desist order or of the court order or the order to pay the penalty, while the order is still in effect, the commissioner may, after hearing, suspend or revoke the license or certificate of that person for a period not exceeding one year; provided, however, no such proceeding shall be based upon the subsequent violation unless the same was committed or continued after the date on which the order imposing the penalty pursuant to the preceding paragraph became final.
The hearings provided by this section shall be conducted in accordance with the Administrative Procedure Act, and the commissioner shall have all the powers granted therein.
The person shall be entitled to have the proceedings and the order of the commissioner therein reviewed by means of any remedy provided by Section 12940 or by the Administrative Procedure Act.
790.08. The powers vested in the commissioner in this article shall be additional to any other powers to enforce any penalties, fines or forfeitures, denials, suspensions or revocations of licenses or certificates authorized by law with respect to the methods, acts and practices hereby declared to be unfair or deceptive.
790.09. No order to cease and desist issued under this article directed to any person or subsequent administrative or judicial proceeding to enforce the same shall in any way relieve or absolve such person from any administrative action against the license or certificate of such person, civil liability or criminal penalty under the laws of this State arising out of the methods, acts or practices found unfair or deceptive.
790.10. The commissioner shall, from time to time as conditions warrant, after notice and public hearing, promulgate reasonable rules and regulations, and amendments and additions thereto, as are necessary to administer this article.
CHSWC Audit Study Advisory Committee
Saul Allweiss, Republic Indemnity
Julianne Broyles, California Chamber of Commerce
Mark Gerlach, California Applicants’ Attorneys Association
Luisa Gomes, Preferred Works and California Association of Service Organizations
Pat Henning, California State Senate Industrial Relations Committee
Mark Johnson, DWC Audit Unit
Lori Kammerer, Californians for Compensation Reform
Joel Laucher, Department of Insurance, Consumer Services Division
Joseph E. Markey, California Self-Insurers Association
Lisa Middleton, State Compensation Insurance Fund
Michael Nave, Alliance of American Insurers
Clea Powell, Kaiser Foundation Health Plan
Peggy Sugarman, Division of Workers’ Compensation
Robert Vines, California Applicants’ Attorneys Association
Willie Washington, California Manufacturers Association
Mark Webb, American Insurance Association
Doug Widtfeldt, Association of California Insurance Companies
Edward C. Woodward, California Workers’ Compensation Institute
Casey L. Young, California Division of Workers’ Compensation
Research Questions for Audit Study
What is the purpose of the audit function of the Division of Workers’ Compensation?
Is it to encourage proper claims handling and to ensure prompt delivery of proper benefits to injured workers?
Does the current audit process work to improve claims administration and how could this be done more effectively?
Are there ways to improve the penalty structure that would make the Audit process more effective at improving system performance? What constitutes ‘unfair practices’ and how should these cases be pursued? Why has the $100,000 penalty never been applied?
What can the audits tell us about the overall performance of the system? How can changes in system performance since the introduction of the audit program be measured?
Can an analysis be designed that would use current data to estimate system performance? Can this be set up to be run each year? How accurately can we know current performance? That is, what is our confidence interval for each estimate of system wide violations? Is the audit program the best way of evaluating system performance?
Are we auditing the correct performance measures?
If not, which performance measures should be audited? What should be deemed "adequate performance"?
Are there unnecessary administrative complexities which tend to interfere with insurers providing benefits in a timely manner?
If so, what are they? How can these be mitigated or eliminated?
Could the audit function provide a mechanism by which administrators at various levels could be made aware of undue administrative complexities?
Benefit Notice violations represent 50% of the citations issued by the DWC Audit Unit. Does this indicate a problem with the Benefit Notice process? If so, what action should be taken?
Are these violations an indication of inadequate claims handling procedures? Is the Benefit Notice program effective? Is it too cumbersome?
Within the DWC Audit process, what is the definition of the term ‘unpaid compensation’?
Are these short delays that would have been paid? Overlooked a long time, but would have been paid? Would never have been paid?
What should be measured that currently cannot be measured?
Could these measurements be provided by the current DWC computer system or by the planned DWC Workers Compensation Information System?
What should be the roles of the Department of Insurance and the Division of Workers’ Compensation regarding audit and enforcement of workers’ compensation insurance requirements, and how should these roles be clarified?
What are the current DWC audit procedures for selecting insurers and self-insureds for audit? Are those procedures sufficient to yield findings representative of the industry?
What audit data is currently available electronically? On paper? How are claim years for each audit chosen?
Given the appropriate audit procedures, what is the optimal number of audits that should be conducted each year to monitor and improve system performance?
How many auditors would be necessary to fulfill this objective?
AUDIT PROGRAMS IN OTHER STATES
ARIZONA
Contact: Ingrid Smith, Industrial Commission of Arizona, (602) 542-4661
Documentation: Training manual including labor code requirements and regulations
Arizona does not have a formal audit program although they do perform small audits of Self-Insureds as part of the licensing agreement.
They are able to review carrier performance by receiving copies of every notice that is mailed to a claimant by an insurance company. These notices are reviewed for accuracy.
Arizona is proactive in that they notify the carrier when an initial claim is filed and remind them of their obligation to respond within 21 days. The computer flags claims that do not receive a timely response and the carrier is contacted and urged to respond immediately.
The Industrial Commission of Arizona provides regular training of workers' compensation policies and procedures for claims professionals. They provide a training manual that contains a copy of their labor code, Rules of Procedure for Workers' Compensation Hearings, correct claims handling procedures, and sample forms.
COLORADO
Contact: Dee Hyslop, Carrier Practices Unit (303) 575-8822
Documentation: The Code of Colorado Regulations; Prototype of Compliance Review Summary Report; Colorado Workers' Compensation Act
Colorado's audit program is under the purview of the Carrier Practices Unit within the Division of Workers' Compensation. Created in 1991, it has been active since 1994 and places strong emphasis on education rather than penalty. They perform audits based on the number of claims filed and focus mainly on the "Big 8" insurance companies which represent 3/4 of the market share.
When audited, a carrier is asked to provide all requested files or copies of requested documentation. The issues to be considered during an audit includes:
- A comparison of the date or receipt of the Employer's First Report of Injury or Workers' Claim for Compensation form and the date of the admission or Notice of Contest.
- The calculation of average weekly wage
- The calculation of compensation benefits
- The date of each payment of compensation to ensure that benefits are paid timely and regularly
- A comparison of the medical billing date and the date of payment
- Compliance with procedures for contesting liability for medical payments or for returning medical billings due to insufficient data
- Modification, termination or suspension of benefits
- Service of documents
After each audit, the carrier is provided with a Review Summary Report that details the violations and provides recommendations to correct identified problems.
OREGON
Contact: Jennifer Flood, Compliance Section (503) 947-7665
Documentation: General description pulled from internet.
Ballantyne, Duncan S. and Dunleavy, James F., Workers' Compensation in Oregon, and "Workers' Compensation in Oregon. Administrative Inventory", Workers Compensation Research Institute.
The workers' compensation system in Oregon is administered through the Department of Consumer and Business Services (DCBS).
The workers' compensation function in Oregon is substantial when compared with other states. The agency is both very large and very active. The division's Compliance Section enforces mandatory-coverage laws, investigates workers' claims against uninsured employers, audits claims-processing performance by insurers and self-insurers and imposes penalties, certifies MCOs, certifies claims examiners and vocational rehabilitation counselors, authorizes self-insurance and vocational rehabilitation organizations, and audits special-fund reimbursements. In 1994, the Compliance Section had 70 positions.
The Field Audit Unit audits the claims-processing performance of insurers and self-insurers to ensure that benefits are paid promptly and that accurate reports are made to the DCBS. The unit conducts three types of audits: an automated quarterly audit, based on insurers' reports, in which penalties are imposed for substandard performance; an audit in which only training and technical assistance are provided; and a full-fledged on-site review, in which penalties are imposed for substandard performance.
In 1994, 85 percent of injury reports, 88 percent of initial payments, and 96 percent of initial claim closure reports were made in a timely way. Public officials cite three features of the system that account for these results: measuring insurers' and self-insurers' performance against stated standards (80 percent of reports and payments made on time), penalizing those who fall below standards, and conducting periodic educational reviews and full compliance audits to verify self-reported performance.
FLORIDA
Contact: Fred Becknell and Vernon Rollins, Bureau of Monitoring and Audit (850) 488-2031
Documentation: Florida Statutes Chapter 440.20 (Time for payment of compensation; penalties for late payment); Chapter 440.185 (Notice of injury or death, reports, penalties for violations); Chapter 440.13 (Medical services and supplies, penalty for violations, limitations); Chapter 440.15 (Compensation for disability); Florida Department of Labor and Employment Security 1998 Dispute Resolution Report.
The Bureau of Monitoring and Audit under the umbrella of the Florida Department of Labor and Employment Security performs audits of workers' compensation carriers to assess the timely delivery of benefits to Florida's injured workers. They are mandated to audit every carrier once every three years and have a target goal of performing 100 audits per year. The core functions of the Bureau of Monitoring and Audit are:
- Overall monitoring and auditing of carrier performance
- Certification of the annual paylag report
- Monitoring accuracy of benefit payments; initiating intervention efforts when appropriate
- Establishing permanent total cases eligible for Division-paid supplemental benefits
- Providing technical assistance to customers through telephone contacts and training and audit workshops
Carriers writing workers' compensation plans in Florida are selected for audit each year by taking into account complaints and the advice of the audit specialists. Audit specialists are assigned 20 to 40 carriers, which they continually monitor for performance.
During an audit, the audit team reviews a random sample of current files within the last 12 months. Auditors look at timely payment of medical bills, timely payment of compensation, and timely filing of required reports.
Upon completion of an audit, a report is written and the carrier is provided the opportunity to appeal. However, appeals are not common. The carrier is assessed penalties and fines but is allowed to waive payment pending the result of a reaudit the following year. If the carrier fails the audit the second year, then it must pay the penalties from the first audit as well as any additional penalties found in the reaudit. A carrier fails an audit when it fails to meet the standard performance standard of 90% for payment of compensation or payment of medical bills. When a carrier fails two audits in a row, it is certified for a third audit the following year. If the carrier fails the third audit, the Department of Insurance can revoke its license.
Collected penalty money is deposited in a trust fund to pay the operating costs of the Division.
Carriers in Florida are expected to meet designated performance standards in certain categories. The minimum performance standard is 90%. For example, the statutory and rule minimum performance standard for timely initial payment of compensation is 90%. The average industry performance of this category in Fiscal Year 1997/98 was 90.7%. The minimum performance standard for Timely Submitted Reports is also 90%, however the industry average in Fiscal Year 1997/98 was merely 60.8%.
The Bureau of Monitoring and Audit designed an Automated Carrier Performance System, an automated tool designed to help track and monitor carriers. The system generates monthly reports that measure individual carrier performance against the industry standards in 10 categories. These categories include but are not limited to: initial indemnity payments, timely submitted reports, and return-to-work rates
In addition to its audit function, the Bureau of Monitoring and Audit performs training workshops for carriers. Upon request, a training workshop can be held at an individual carrier at their expense. Training and education is also part of the on site audit.
TEXAS
Contact: Veronica Lane, Compliance and Practices (512) 440-3727
Documentation: Compliance and Practices slide-show presentation; statutory language, organizational chart, System Data Report generated monthly that outlines some of the Division's performance measures defined by the Legislature
The Division of Compliance and Practices under the Texas Workers' Compensation Commission monitors carrier performance in Texas. This Division contains four units. They are the Office of Investigations which investigates fraud allegations (15 investigators), Compliance Information Management (5 data specialists), Performance Review & Enforcement Strategy (1 planning assistant, 17 auditors and 1 ad tech) and the Carrier Administrative Review Evaluation (5 auditors and 1 ad tech).
The primary functions of the Division are (1) monitoring compliance and (2) investigation of fraudulent behavior by system participants. Although penalties are a component of Texas enforcement, their favored approach promotes communication, cooperation and education
The Division conducts three types of audits, Reactive, Proactive, and Targeted.
Reactive auditing is complaint-driven. The division receives hundreds of referrals every month from employees, employers, carriers, health care providers and attorneys as well as from field offices and other state and federal agencies.
Proactive auditing is an audit process based on random sampling of claims or medical bills selected by the Commission. Using statistical procedures, this method allows the Commission to project compliance across a carrier's entire population of claims or medical bills. Indemnity audits, conducted on a random sample of claims, focus on issues relating to the timely and accurate delivery of benefits including health care provider and employer reporting duties. Medical audits, conducted on a random sample of medical bills, focus on medical benefit delivery such as medical bill payment and utilization review by carriers as well as preauthorization compliance. Carriers are selected for a medical or indemnity audit based on performance factors, such as benefit delivery/reporting performance, dispute resolution practices, system impact, and referral activity. . The Division's goal for onsite indemnity audits per year is 30. It's goal for medical audits is 36. However, the medical audit team currently has three staff and the capability of performing only 28 audits per year.
Targeted auditing is more strategic than the other methods and uses Commission data to identify possible violations. Once potential violations have been identified, case reviews are conducted to confirm the violation and then appropriate enforcement actions are taken.
Once a violation has been found, there is an opportunity for the violator to discuss these violations with staff prior to assessing penalty amounts. There are two programs for this purpose: The Voluntary Compliance Conference and the Compliance Plan Program.
The voluntary Compliance Conference is an opportunity for the violator and Division staff to get together and discuss the violation prior to the Commission taking formal action. At the conclusion of the conference, the violator is offered a reduced penalty amount if the violator is willing to sign a standard settlement agreement in which the violator:
- admits to committing the violation;
- agrees to improve compliance
- agrees to pay reduced penalty amount
Voluntary Compliance Conferences have proved so successful in Texas that the concept was expanded to cover all system participants and al types of violations. Is features have been adapted into other programs such as the Compliance Plan Program.
The Compliance Plan Program is a voluntary program whereby carriers audited by the Commission enter into a compliance plan that addresses problems found by the audit team. The program was created out of a realization that many carriers were using Commission audits as their only compliance review. The Division provides evaluation tools for carriers to measure their compliance and to identify problems proactively and allows self-audits to be validated by staff to determine improvement and compliance.
In response to recent hearings before the House Business and Industry Subcommittee on Insurance Carrier Practices, the Division of Compliance and Practices is developing a method to perform compliance audits that focus on overall compliance rather than specific carrier compliance. These audits would be conducted on an annual or biennial basis to allow compliance to be measured over time. The results of these audits could also help determine how resources should be allocated by quantifying what areas have the poorest compliance by assessing the compliance of carriers, employers, and health care providers.
WISCONSIN
Contact: (608) 266-3149
Documentation: Labor Code and Regulations. "Workers' Compensation in Wisconsin - Administrative Inventory," Workers Compensation Research Institute.
In Wisconsin, workers' compensation carriers are monitored by the Office of the Commissioner of Insurance. Wisconsin does not perform physical audits of claim files. Instead, they receive copies of all notices sent to injured workers and review these notices for accuracy and timeliness. Claim information is entered into a computer system on receipt of the first report. The computer system generated inquiries when deadlines are not met. Where violations are found, assessments are made in a manner and amount set by the Wisconsin labor code. In evaluating whether payments of compensation and reports made by insurance carriers and self-insured employers are prompt and proper, the department considers the following performance standards:
Payment of first indemnity: Insurers are expected to make 80% or more of first indemnity payments within 14 days following the date of injury or the last day worked after the injury before the first day f compensable lost time. The Workers' Compensation Division publishes an annual report on the performance of individual insurers and self-insured employers. The division contacts employers and insurers who do not meet timely payment standards. Meetings may be scheduled to discuss problems in complying with the standards and to develop strategies for improving performance. Division staff also may be assigned to work with targeted employers and insurers to provide direct assistance and improve communication. The division is active in monitoring payment. All payments are examined for both correctness and timeliness, and apparent delays in payment are investigated and pursued if no reasonable excuse is provided. If an employer's or insurer's inexcusable delay results in late payment of compensation, the delayed benefits are increased by 10%, with the responsible party bearing the cost. If there is no response to a request for a penalty payment, the division issues an order on default. Interest is charged until payment is made.
First report of injury: Insurers are expected to file 70% or more of reports within 14 days of the date of injury or the last day worked after injury before the first day of compensable lost time.
Correct and complete names: Names of self-insured employers on reports filed with the department must be correct and complete. The name of an insurance group is not a substitute for the name of the individual company insuring the risk. The name of an insurance service company is not a substitute.
Penalty frequency and severity. Wisconsin has a stiff penalty for malice or bad faith concerning failure to report an injury, failure to make payments, unreasonable denial, or improper suspension or termination of benefits which prompts many employers and insurers to pay many claims voluntarily and issue few denials. On determination of malice or bad faith, the division can award an amount that it considers just, not to exceed the lesser of 200% of the total compensation due or $15,000. A late-payment penalty can be assessed in addition to a bad-faith penalty. Several insurers sometimes issue workers one weekly benefit check within the fourteen-day time frame without accepting liability for the claim in order to avoid penalties. Technically, this satisfies the requirement for on-time payment. On receipt of medical information, the claim then is either accepted or denied. Insurers indicate that this "provisional pay" concept encourages prompt decisions without forcing denials, which can increase litigation in the system. Public officials note that payments continue uninterrupted in the vast majority of these cases.
Description of Current Audit Selection Process
Random and Non-Random
The terms ‘random’ and ‘non-random’ are used in two different ways in the current audit process:
- Audit location selection from among all locations
- Selection of files from among all files at a selected location
Audit location selection
Random Audits:
Definition of ‘location’: As used by the Audit Unit, three dimensions define a location:
- Geography -- the address at which claims are adjusted. If a single firm has ten adjusting offices, each office is considered a separate location.
- Firm -- The highest level of the claims examining firm (e.g., Allied Group Insurance location 1009 covers the following entities, all are considered a single location: Allied Mutual Insurance, Allied Property & Casualty Insurance Co., Amco Insurance Company, and Depositors Insurance Co.)
- Function – Each function (TPA, self-administered-insurer, Self-administered/Self-insured) defines a separate location. Consequently, a self-insured insurance company that self-administers its own claims, adjusts its insureds’ claims, and acts as a TPA for another insurer or self-insured firm, would be considered 3 separate locations for the purpose of auditing.
For the purposes of selecting locations for random audit, each unique combination of geography, firm, and function is considered a location. Each location is given an equal chance of being selected.
The chance of being selected is not affected by the number of claims at a location, or the function of the location. For example, an insurer that self-insures/self-administers its own workers comp with less than 10 claims, and has a large insurance operations which it also administers at that location with more than 10,000 claims would have the same chance of being audit for the 10 claims as it does for the 10,000 claims.
The following table shows the distribution of claims among claims adjusting locations that could have been selected for the 1997 audit. The figures are based on the total number of claims reported on the 1995 and 1996 Annual Report of Inventory.
Figure 1: Distribution of claims locations by number of claims
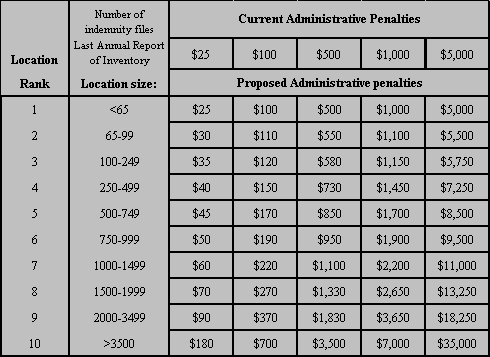
Even though each location has the same chance of being selected for a random audit, the vast majority of claims are concentrated in the largest locations. The smallest 40% of locations have only 3% of all claim files. Or put another way, the largest 10% of locations average 16,000 claims per location subject to audit in 1997. The smallest 10% averaged 18 claims per location. However, each location had the same likelihood of being audited. The largest locations were 1000 times larger, but no more likely to be audited.
The chance of being audited on a random basis in 1997 was less than 5%. Based on 1997 numbers, any location could expect to be subject to random audit approximately once every 21 years.
Note: There were 665 unique locations reporting for the 1995 and 1996 claim reporting years. Of these, 57 reported no claims for both 1995 and 1996 and therefore were not subject to audit in 1997. This left 608 locations reporting at least one claim for the 1995 and 1996 calendar years and thus subject to a random audit. The Audit Unit conducted 29 random audits in 1997.
Non-Random Audits:
Audits are also targeted on the basis of:
- Complaints
- Past audit performance
Locations are rated based on the frequency and seriousness of complaints. Each complaint is assigned a certain number of points based on the seriousness of the violation reported.
The points assigned range from
1 point for violations under 10111.1(a) with penalties up to $100. (example, failure to pay 10% self imposed increase with late payment of indemnity)
5 points for violations under 10111.1(b) with penalties up to $500 (examples, failure to list full claim information on claim log, failure to supply claim logs to Audit Unit within specified time frames)
10 points for violations under 10111.1( c ) with penalties up to $1000 (example, failure to pay permanent disability indemnity based on a reasonable estimate of PD)
50 points for violations under 10111.1 (d) with penalties up to $5,000 (example, unsupported denial of a claim)
If a violation is reported by a WCAB judge/referee, the points are multiplied by 10.
The total number of points assigned to a claims administrator at an adjusting location is compared to the total number of claims reported at that location. The claims administrators are ranked on the basis of the ratio of weighted complaints to caseload size. The Audit Unit then selects the highest-ranking locations for investigation.
In 1997, 10 locations were targeted for a non-random audit.
Collection of complaints for the purposes of targeting
Driving the targeting process is development of information in the form of complaints generated from various sources. The efficiency and accuracy of the targeting process are to a large extent dependent on the success of the DWC in generating a predictive picture of claims practices through complaint monitoring. However, this process depends on:
- Collecting sufficient numbers of complaints
- Collecting complaints early in the claims process
- Collecting complaints in an unbiased manner.
On these criteria, the current DWC methods appear to fail.
Sufficient numbers:
DWC has several sources for complaints. The most important are WCAB judges and I&A officers. Judges’ complaints are weighted more heavily under the Audit Unit system. One WCAB area supervisor estimated that 10%-15% of cases heard by judges include LC 5814 violations, which should be referred to Audits. This translates to 1,000 to 3,000 observed violations per year. However, it does not appear that the total number of complaints, from all sources, referred to the Audit unit exceeds 350-500 in any year., Data from the Audit Unit for the most current Fiscal Years confirms this issue (see Table 2). Very few complaints are reaching the Audit Unit from the WCAB, and even fewer from I&A.
Table 2: Sources of Complaint Referrals to Audit Unit
Percent of all complaints, both FY |
FY 97/98 |
FY 96/97 |
Source of Complaint Referral |
6.0% |
22 |
59 |
WC Judge |
1.1% |
2 |
13 |
Rehab Unit |
23.3% |
97 |
219 |
Injured Worker |
6.0% |
16 |
65 |
Applicant's Attorney |
5.3% |
11 |
61 |
I & A Unit |
33.2% |
142 |
307 |
Medical Treatment Provider |
19.4% |
85 |
178 |
Medical-Legal Provider |
1.1% |
1 |
14 |
Medical Billing Service |
4.1% |
15 |
40 |
Other |
0.5% |
7 |
No entry given to show source |
|
391 |
963 |
TOTAL |
Note: The "other" includes Audit Unit personnel, relatives of injured worker, DEU, employers, and anonymous complainants. Coding of complaints began in FY 96/97 and included some complaints submitted earlier, but not coded.
Early in the claims process
:Complaint referrals generated by the WCAB are likely to occur long after claims have been filed. With hearings in the WCAB occurring years into a claim, and the process of referral and analysis by the Audit Unit adding another year. The timeliness of this information is questionable. Early warning of possible problems should be an objective of the targeting process. I&A officers have thousands of contacts each month with injured workers, many of which involve problems with claims handling by the insurer. These issues often arise early in claims and would serve as an earlier warning system on problems developing at claims handling locations. However, available data on the I&A Unit indicate that even during the two years when these referrals were a priority for I&A, only a couple hundred violations on average are collect this way each year (see Table 3). There are also appear to be no clear guidelines within I&A on what constitutes an appropriate complaint for referral. As indicated by Table 2, referrals from I&A have dropped dramatically. Even assuming that all complaints from injured workers are generated through the assistance of I&A, barely one hundred referrals per year are being generated through I&As 10s of thousands of contacts.
Unbiased Collection:
Since claims at individual claims locations are often geographically specific, differences in the complaint process across WCAB and I&A offices will have an important effect on the relative frequency of complaints against different claims locations. This will lead to reduced effectiveness and efficiency in the targeting process and an unfair auditing burden being imposed on locations situated in high referral areas. There appears to be a lack of consistent supervision and training in the area of complaint referral both at the WCAB and I&A. The following table (Table 3) shows the complaint referrals by I&A offices for the time period 1994 and 1995. This shows substantial differences between areas. While some differences can be explained by the size of the offices, even very large offices such as LA and Van Nuys apparently referred very few claims for audit.
In addition, because medical providers will be localized geographically, and because medical providers are the dominant compliant source, audit targeting could again be driven by a few localized complainants. Complaints from medical providers, while legitimate, may focus the attention of the Audit Unit on claims administrators’ with aggressive bill review suppliers, rather than the insurers who are failing to deliver benefits to injured workers accurately and in a timely manner.
Table 3: Information and Assistance referrals to the Audit Unit
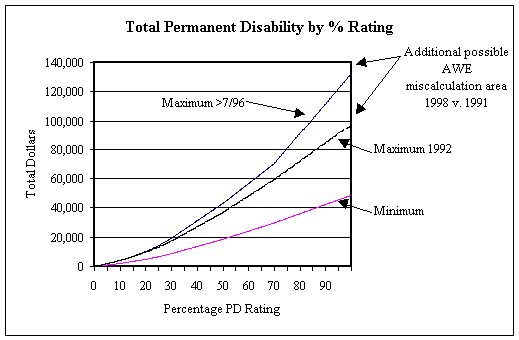
Selection of files at audit locations
At each location selected for audit, files are selected for review on both a targeted and random basis.
Targeted files:
All files at a selected location that were the subject of one or more complaints are separately targeted for audit.
Random files:
Once a location is identified for audit, the location submits claim logs identifying all claims subject to audit. These claims are listed separately by:
- Medical-only
- Indemnity
- Denied
Depending on the size of a location, all claims or a sample of claims in a category are identified by the Audit Unit. If a sample is used, the claims are assigned numbers and randomly selected.
In 1997, 2,190,314 files were potentially subject to audit. These represent all claims reported during 1995 or 1996 at all identified claims administering locations.
Of these claims,
- 8504 claims were randomly selected for audit. This represents approximately 0.4% of all claims reported for the period subject to audit.
- 89 additional files were selected for audit on the basis of complaints.
Complexity of the Benefit Delivery Process
Calculating workers’ compensation indemnity benefits and producing the supporting notice requirements are complicated processes. The purpose of this section is to provide a brief description of some system complexities which may contribute to the benefit delivery results reported in 1997 Audits – A Report to the California Legislature on Claims Handling Practices of Workers’ Compensation Administrators.
The attached Indemnity Benefit Calculation Comparison Chart summarizes major benefit calculation considerations and provides statutory cites to which this section will refer.
Both late and non-payment of benefits due injured workers or their dependents are identified by the Division of Workers’ Compensation (DWC) through the compliance audit.
Included as part of its findings, the DWC reported in its annual report that 508 Notices of Compensation Due for $455,401.53 were issued in 1997. (Refer to Appendix J for a table and full description of Notices of Compensation Due.) Compensation found to be due but unpaid included:
- Temporary Disability (TD) and Salary Continuance – paid instead of TD – for a total of $152,618.80.
- Permanent Disability (PD) for a total of $197,654.35.
- Vocational Rehabilitation Maintenance Allowance (VRMA) for a total of $17,239.25.
- Self-Imposed Increases (SII) as described Labor Code Section 4650(d) for a total of $73,091.88.
- All other unpaid benefits to injured workers including penalties (Labor Code §5814) and interest for a total of $14,797.25.
In addition, DWC compliance auditors documented late payments to injured workers and their dependents. For example, late first Temporary Disability payments were found in 21% of the reviewed files requiring a first TD payment for a total of 369 late first payments. Two hundred-six (206) files – or 31% of the files with exposure – contained late first Permanent Disability payments. Two hundred-fourteen (214) files or 16% of the files with exposure for additional indemnity benefits contained a late indemnity payment subsequent to the first payment.
On the flip side, representatives from both the Division of Workers’ Compensation (DWC) Audit Unit and claims administrators advise that overpayments to injured workers also occur. Even though the extent of over-compensation is neither monitored nor measured, over-payments suggest that some benefit delivery deficiencies found in audits may result from errors. One then must ask what is satisfactory performance, how is it measured and what is an acceptable level of error? Before anyone attempts to answer such questions, studying any characteristics of the workers’ compensation system that may impact the quality of benefit delivery is necessary.
An overview of how a claims administrator determines the major types of benefits due to an injured worker or a dependent provides some evidence of system complexity. When a worker sustains an injury or illness entitling him or her to indemnity benefits, the claims administrator must consider three different types of benefits when calculating payments:
I. Temporary Disability (TD)
II. Vocational Rehabilitation Maintenance Allowance (VRMA)
III. Permanent Disability (PD)
Various factors affect the calculation and amount of compensation paid directly to the worker when providing one or more of these benefit types. Factors include:
- Injury Year as it determines the minimum and maximum weekly benefit levels for an injured worker. Minimum and maximum weekly rates vary from one type of benefit to another.
- Temporary Total Disability benefits paid two or more years after the injury date (Labor Code §4661.5).
- Average Weekly Earnings (AWE)/Wage determination in accordance to statute and complex case law.
- Proper attachment of self-imposed increases (SIIs) to portions of late paid temporary and permanent disability benefits.
- Review of the qualified injured worker’s benefit entitlement in response to a Permanent and Stationary (P&S) date when in rehabilitation.
- Determination of attorney fees to be withheld from VRMA if a qualified injured worker is represented.
- Payment of actual PPD or a reasonable estimate upon each termination of an injured worker’s TD and then adjustment of PPD benefits (retroactive and prospective) if the extent (seriousness) of permanent disability changes.
I. Temporary Disability (TD)
Indemnity Benefit Calculation Comparison Chart & Addendum 1A. Minimum Temporary Disability Weekly Rate
Calculating the minimum temporary disability weekly rate has become more complex since 1989 reform. Depending upon injury year, the TD rate equals average weekly earnings for the lowest wage earners. (Refer to Addendum 1.) Previously, the weekly TD rate defaulted to a fixed minimum weekly rate.
B. Maximum Temporary Disability Weekly Rate
Subsequent to 1989 and five benefit level increases, two-thirds of an injured worker’s average weekly wages over a certain dollar amount continue to be provided as TD up to "maximum" weekly levels. However, the "maximums" have increased step by step from $224 per week to the current $490 depending upon the injury year. (Refer to Addendum 1.) As a result, tasks associated with proper benefit calculation are more complicated:
1. Increased Importance of Wage Statements
When average weekly earnings (AWE) are not clear, a claims administrator often will send the employer and injured worker a form and ask each to document the worker’s wages. The "form" typically is called a wage statement. The employer, including previous employers, may complete the form. Often an injured worker provides other documentation instead of the form including prior years’ W-2 documents.
Since the last five TD benefit level increases, some claims administrators reportedly have had to use the wage statement verification process more extensively to precisely document AWE. Prior to 1990, establishing AWE sufficient to generate the "maximum" TD rate was fairly simple in many instances as the salary threshold to generate it was lower. Occasionally when an injured worker’s AWE could not be determined to the exact dollar, the amount of substantiated pre-injury earnings was sufficient to justify payment of the maximum TD weekly rate without any further investigation. However, the same amount of substantiated AWE today may not produce a maximum TD rate thereby requiring additional investigation to calculate the correct TD weekly rate.
And, determining the AWE at time of injury subsequent to 1989 reform legislation has become increasingly important even for the injured worker with earnings sufficient to produce the maximum weekly rate at time of injury. The claims administrator might need the AWE documentation to assist with recalculation of the TD weekly rate for future payments that might occur two or more years from date of accident. (Refer to Number 2 – Labor Code §4661.5 Increases – for further discussion.)
A number of considerations can influence the AWE in addition to wages such as raises, number of hours worked, and the market value of other advantages provided the worker such as room and board. While developing documentation through the wage statement process usually is relatively simple for a salaried worker, the same may not be said for an injured worker paid on an hourly, piecemeal, part-time or seasonal basis. In addition to the variances due to overtime and seasonal demand, the employee may have worked for a number of employers for the year prior to the injury. Requesting the wage statement information from the employer(s) and employee, receiving the information, re-calculating the TD rate based on information that may be conflicting or confusing and then paying TD present ample opportunities for mistakes and delays.
2. Labor Code §4661.5 Increases
If an injured worker is paid temporary total disability two or more years from the date of accident, he or she is entitled the TD rate in effect at time of payment if the recalculation produces an increase.
Recalculating temporary disability for maximum wage earners when paid two years from the date of injury has been required for a number of years even prior to 1989 reform legislation. However, awareness of the need for Labor Code §4661.5 TD recalculations has become all the more important. The five increases of the maximum TD rate have multiplied the number of times a claims administrator must recognize the need for checking the weekly rate before payment of TD if:
- an injured worker’s injury occurred two or more years ago; and,
- AWE previously produced a maximum weekly TD rate.
C. Late Temporary Disability Payments – Self-Imposed Increase (SII)
In addition to Labor Code §5814 increases awarded to an injured worker by a Judge for an unreasonable delay, a worker with an injury date on or after January 1, 1990, may be entitled to an automatic benefit increase (temporary and permanent disability per Labor Code §4650). The 10% augmentation is commonly referred to as a "self-imposed increase" or SII. The claims administrator may add a 10% SII to the portion of a late temporary or permanent disability payment after a number of considerations:
- Recognizing that the late payment has occurred.
- Verifying that the injured worker has filed a claim (DWC-1 form) and determining the filing date per Labor Code §5401.
- Determining if an insured employer caused the delay under circumstances as described in Labor Code §4650(e) and then coding the SII payment appropriately to identify employer delay.
- Coding the SII portion of the TD (or PD) check so the 10% increase is tracked separately for reporting purposes.
D. Temporary Disability Payments – Superior Court Orders to Withhold for Child Support Judgment
While not included as an item on the Indemnity Benefit Calculation Comparison Chart, a Superior Court judge can sign an order requiring a claims administrator to withhold up to 25% of an injured worker’s TD to satisfy a judgment for unpaid child support. Anecdotal evidence suggests that the frequency of these orders is increasing. Plus, confusion occurs over what benefits are subject to the withholding order. The tasks associated with paying the net benefits to the injured worker, tracking the withholdings and maintaining the records have created another dimension of calculations and bookkeeping.
II. Vocational Rehabilitation Maintenance Allowance (VRMA)
Indemnity Benefit Calculation Comparison Chart & Addendum 1
- Vocational Rehabilitation Maintenance Allowance (VMRA) versus Vocational Rehabilitation Temporary Disability (VRTD)
Legislative reform created a new benefit for injuries on or after January 1, 1990 – Vocational Rehabilitation Maintenance Allowance – to replace Vocational Rehabilitation Temporary Disability (VRTD). Unlike VRMA, the P&S date had little impact for pre-1990 injuries when benefits shifted from medical TD to VRTD other than the potential withholding of attorney fees:
- An injured worker’s weekly VRTD rate remained the same as medical TD.
- An injured worker’s VRTD payments did not count toward a monetary cap (VRMA paid for injuries on or after January 1, 1994, typically counts against a $16,000 cap.)
VRTD was an extension of medical TD and VRTD even qualified for the bump two years after injury per Labor Code §4661.5 if average weekly earnings were sufficient.
- Entitlement to Payments While in Vocational Rehabilitation
While methods for calculating VRMA are similar to medical TD, the weekly VRMA benefit has a weekly maximum of $246 per week for all injury years on or after January 1, 1990. As mentioned previously, the P&S date since 1990 has great significance to the injured worker and to the claims administrator responsible for calculating the benefit. (Refer to Addendum 1.)
The amount of money in an injured worker’s check while entitled to VRMA depends upon a number of factors:
- PD Supplements
- Attorney Fees
- Caps/Late Payments/Delays
An injured worker may supplement his VRMA when the cap of $246 per week produces a weekly benefit less than his or her medical TD rate. Upon request, the injured worker is provided PD supplements – assuming PD is due – bringing the weekly rate to the medical TD level. At the time of the Award, the employer/claims administrator will seek credit for the PD supplement portion paid.
Attorney fees might be withheld from the VRMA portion of the payment to the injured worker – typically around 12%. The practice of withholding attorney fees upon request pre-dated 1989 reform legislation.
New limitations were placed on vocational rehabilitation services and benefits including a $16,000 cap for injuries on and after January 1, 1994. However, exceptions to the limitations – including the weekly VRMA maxim of $246 per weekly and the $16,000 cap – are possible.
The 1989 reform legislation created Labor Code §4642 to address an employer’s – including a claims administrator’s – delay in the provision of vocational rehabilitation services. The effect of an employer’s late provision of rehabilitation services as described in Labor Code §4642 depends upon the injury year:
(a) For injuries on or after 1/1/90 but prior to 1/1/94, payment of VRMA is made at the medical temporary disability rate for the period of delay.
(b) For injuries on or after 1/1/94, payment of VRMA is made at the medical temporary disability rate during the delay. Furthermore, the VMRA payments required under Section 4642 and costs attributable to the delay are not counted against the $16,000 cap. And, if an insurer was primarily responsible for the delay as described in Labor Code §4642, the increased costs are paid against its expenses.
Additionally, while an injured worker is not entitled to a 10% SII per Labor Code 4650 when VRMA is paid late, it would apply to the late portion of a PD supplement assuming the DWC-1 (claim form) has been appropriately filed.
The multiple considerations – including injury year – when determining the amount and type of benefit(s) due, appropriately compensating for late payments and delays and properly coding for "caps" and insurer expenses can be confusing.
III. Permanent Partial Disability (PPD)
Benefit Calculation Comparison Chart & Addendum 2A. Payment of PPD Upon Termination of TD
If an injury causes permanent disability, the claims administrator per Labor Code Section 4650 must begin paying the permanent disability within 14 days after the last payment of temporary disability. Often the injured worker’s condition is not P&S when temporary disability terminates, so the extent of disability is not necessarily known. The claims administrator begins paying its reasonable estimate. Permanent disability accrued but not paid at time of a DWC compliance audit is designated as unpaid compensation even if the PD will be paid later.
Termination of TD is not a single occurrence in a number of claims. An injured worker may have many broken periods of temporary disability when medical TD starts and then stops. Each time TD is terminated, the claims administrator must begin PD payments if due per Labor Code §4650. Also, if a claims administrator receives a subsequent medical report establishing actual or probable disability, PPD must be paid retroactively for previous occasions when TD was terminated and PD did not appear to exist. And, the claims handler must determine whether the injured worker is entitled to the start or resumption of PD payments upon termination of VRMA if medical TD is not resumed.
B. Permanent Partial Disability – Weekly Rate/Number of Weeks
Calculation of Permanent Partial Disability (PPD) was significantly impacted by 1989 legislative in two ways: (1) creation of the multiple "maximum "weekly rates; and, (2) the change in the number of weeks of PPD paid.
Both the injury year and the extent – or seriousness – of PPD affect the calculation. While the injury year is a static variable assuming no dispute, the extent of PPD (actual or a reasonable estimate) may change throughout the course of the claim thereby requiring a recalculation of the PPD rate and the number of weeks owed.
1. Prior to January 1, 1991, an injured worker was paid two-thirds of his or her average weekly earnings subject to one minimum and one maximum on the weekly rate. PPD resulting from injuries occurring on or after January 1, 1991 still requires calculation of PPD at two-thirds of AWE.
However, an injured worker with a higher AWE may be entitled to any number of "maximum" disability weekly rates depending upon the level (extent) of adjusted permanent partial disability. Two different maximum weekly PPD rates were created for injuries on or after 1/1/91. Multiple "maximums" were created for weekly PPD payments for injuries on or after 7/1/94. The weekly rates for the multiple "maximums" were increased for injuries on and after 7/1/95 and again for injuries on or after 7/1/96.
For example, an injury subsequent to July 1, 1996 would produce a maximum PPD weekly rate of $160 for an estimated or actual 15% permanent partial disability assuming the injured worker’s AWE was sufficient. If subsequent information indicates an estimated or actual PPD of 25% through 69.75%, the PPD weekly rates should be adjusted to $170. Conversely, if the PPD later is determined to be or estimated at less than 10%, the weekly maximum drops to $140. Any PPD at 70% or more but less than 100% entitles an injured worker to $230 per week for a number of weeks prior to the start of the life pension.
2. Addendum 2 of the Indemnity Benefit Calculation Comparison Chart demonstrates that an injured worker’s weekly rate is not the only fluctuating component when calculating PPD. The number of weeks due also varies depending upon the seriousness of PPD. Although the concept of adjusting the number of weeks of PPD paid for each percent of PPD pre-dated 1989 reform, the number of weeks for the formula changed for injuries on or after January 1, 1992. The formula continued to take into account the cumulative effect of the lower ranges of PPD.
Rather doing the math that includes accounting for the cumulative effect on total weeks to be paid, most claims handlers refer to a chart. However, if the claims administrator goes directly to the "answer" on the chart– total dollar payment – and does not reconsider the weekly PPD rate, total PPD due may be paid at the wrong weekly rate. Regardless of any intent to pay out the all PPD – albeit at the wrong rate – the oversight may result in a Notice of Compensation Due for unpaid PPD due at time of the DWC compliance audit.
In summary, the injury year and the extent of PPD (estimate or actual) affect the weekly PPD rate and the number of weeks of PPD due.
C. Late PPD Payments
An injured worker is entitled to a 10% SII per Labor Code 4650 when PPD is paid late.
Addendum 1
Temporary Total Disability &
Vocational Rehabilitation Maintenance Allowance
For Injuries Subsequent to 12/31/89
Injury Years: |
Average Weekly |
Weekly |
Weekly |
01/01/90 |
$0.01 through $98.00 $98.01 through $112.00 $112.01 through $168.00 .66667 of $168.01 through $339.00 to a |
$98.00 Actual Earnings $112.00 Maximum $266.00 |
$98.00 Actual Earnings $112.00 Maximum $246.00** |
01/01/91 |
$.01 through $126.00 $126.01 through $189.00 .66667 of $189.01 through $504.00 to a |
Actual Earnings $126.00 Maximum $336.00 |
Actual Earnings $126.00 Maximum 246.00** |
07/01/94 |
$.01 through $126.00 $126.01 through $189.00 .66667 of $189.01 through $609.00 to a |
Actual Earnings $126.00 Maximum $446.00 |
Actual Earnings $126.00 Maximum $246.00** |
07/01/95 |
$.01 through $126.00 $126.01 through $189.00 .66667 of $189.01 through $672.00 to a |
Actual Earnings $126.00 Maximum $448.00 |
Actual Earnings $126.00 Maximum $246.00** |
07/01/96 |
$.01 through $126.00 $126.01 through $189.00 .66667 of $189.01 through $735.00 to a |
Actual Earnings $126.00 Maximum $490.00 |
Actual Earnings $126.00 Maximum $246.00** |
| Claim Technicians either multiplies the AWE by 2 � 3 or by .66667 when determining weekly TD or VRMA. When using a decimal, five places are necessary to avoid calculation errors. |
* Subject to Withholding of Attorney Fees
** Subject to Permanent Disability Supplement and an increase to the medical TD rate under Labor Code § 4642. Refer to endnote 7 for Labor Code §4642
Note: Formatting and presentation of statutory benefit levels suggested by Table 14 from Tables and Schedules revised by James T. Stewart from the 1998 Workers’ Compensation Law of California published by Matthew Bender & Company, Inc. Refer to page 964.
Addendum 2
PERMANENT PARTIAL DISABILITY
Note: The PD severity impacts the number of weeks that will be paid at the established PD disability rate.
For Injuries prior to 1/1/92 WEEKS*
Less than 10% 3
10.00% through 19.75% 4
20.00% through 29.75% 5
30.00% through 49.75% 6
50.00% through 69.75% 7
70.00% through 99.75% 8
For Injuries On or After 1/1/92
Less than 10% 3
10.00% through 19.75% 4
20.00% through 24.75% 5
25.00% through 29.75% 6
30.00% through 49.75% 7
50.00% through 69.75% 8
70.00% through 99.75% 9
*Number of weeks for which two-thirds of average weekly earning (subject to a minimum and maximums) are paid for each 1 percent of PPD after taking into account the cumulative effect of lesser PPD ranges.
Example:
A worker injured on March 12, 1996, sustains a PPD that the claims administrator initially estimates at 9% PPD after adjustment for age and occupation. A subsequent medical report from the primary treating physician indicates that his condition is Permanent and Stationary. The claims administrator rates the report and the PPD is now 25.%. AWEs were established at $946. per week.
9.0% PPD equals 27 weeks of PPD@ 140. per week.
25.0% PPD equals 95.5 weeks of PPD @ $164. per week.
Refer to Labor Code §4658 for an explanation of the cumulative effect when determining the number of weeks to be paid.
Analysis of ‘Compensation Due’ for 1997
Statewide Summary
Calendar Year 1997
(1) Temporary Disability |
(2) Permanent Disability |
(3) Vocational Rehabilitation Maintenance Allowance |
(4) Self -Imposed Increase
|
(5) Death Benefits |
(6) Penalty/ |
| $152,618.80 | $197,654.35 | $17,239.25 | $73,091.88 | $0.00 | $14,797.25 |
When unpaid compensation is discovered during a compliance audit, the Administrative Director serves a Notice of Compensation Due on the claims administrator with a copy to the affected employee or dependent per Labor Code §129.
The reported unpaid benefits include only those claims and benefits where liability is not in dispute.
Compensation due includes:
1. TEMPORARY DISABILITY – Unpaid benefits not paid according to Labor Code §4650(a)(c) or in response to an Award per Labor Code §§5800, 5903 and 5950.
Payment is due within 14 days of the employer’s knowledge of injury and disability. The claims administrator is to make subsequent payments every two weeks thereafter on the day designated with the first payment.
2. PERMANENT DISABILITY – Unpaid Permanent Disability as required by Labor Code §4650(b)(c) and Labor Code §§5800, 5903 and 5950.
The first payment of Permanent Disability is to start within 14 days after termination of Temporary Disability. If the extent of PD cannot be determined, the claims administrator must pay its reasonable estimate. Subsequent Permanent Disability is due and then paid every to weeks thereafter on the day designated with the first payment. If the extent of Permanent Disability is not known, a reasonable estimate of the extent must be paid.
Permanent disability also may have been unpaid in response to an Award for permanent disability per Labor Code §5800.
3. VOCATIONAL REHABILITATION MAINTENANCE ALLOWANCE(VRMA) – Unpaid Vocational Rehabilitation Maintenance Allowance not paid per Labor Code §139.5.
Under Labor Code Section 4642, the injured worker is entitled to VRMA at the medical temporary disability rate for the period of time the employer delays the provision of rehabilitation services. Unpaid Labor Code §4642 payments are reported as either unpaid Temporary Disability or VRMA.
4. DEATH BENEFITS – Unpaid death benefits, including burial expenses, due per Labor Code §4702.
5. SELF-IMPOSED INCREASES – Unpaid Self-imposed Increases due under Labor Code Section 4650(d).
Temporary and Permanent Disability benefits paid late are increased by 10% – a self-imposed increase (SII). The reported unpaid SIIs include increases due and payable at time of audit as well as additional SIIs that will be due when the claims administrator pays Temporary or Permanent Disability benefits in response to the Notice of Compensation Due.
6. PENALTY, INTEREST OR OTHER – All other unpaid benefits.
Unpaid penalties (Labor Code §5814) are tracked in this column as well as unpaid interest that was to have been paid in response to an Award (Findings and Award, Stipulated Findings and Award and Compromise and Release per Labor Code §5800).
Any other compensation due an employee or dependent such as reimbursement for self-procured medical treatment or mileage is included.
***
Evaluation of Data and Goals of the Audit Unit
Introduction:
The Audit Unit (AU) of the Division of Workers’ Compensation (DWC) is set up to perform random and targeted audits of locations handling claims adjusting either as part of an insurer, third party administrator, or self-administered—self-insured employer.
The audit process should:
- Evaluate the performance of individual claims administrators
- Encourage improvements in claims administration through incentives and penalties connected with the review
- Monitor the performance of the compensation system across important components of the claims process.
As currently designed, the system accomplishes only the first of these goals with any degree of success. At the same time, half of the violations are for relatively minor infractions of the Benefit Notice requirements suggesting that these may be unnecessarily cumbersome requirements.
The data in the Audit Unit Annual Reports are insufficient to evaluate system-wide performance. However, appropriate data are available and reporting should be changed to facilitate assessment of the system by policymakers and the DWC. A method of evaluation could be developed that would be straightforward to implement by the AU each year. This would give the legislature and the DWC consistent benchmarks against which to compare improvement.
As currently structured, the penalties are unlikely to motivate improved performance. These penalties are too small and too unlikely to be imposed. They burden good performers while not giving adequate incentive to poor performing locations to improve. At the end of this memorandum, we outline a method that could greatly enhance the incentives and improve targeting.
Background:
The AU selects claims administering locations either on a random or targeted basis.
- Random audits are selected by weighting each location by several factors, such as how recently they were audited and how well they performed on their last audit.
- Targeted audits are selected based on complaints submitted to the AU. These complaints are weighted according to the source of the complaint and the seriousness of the issues raised.
Once a location is selected, claims at that location are separated into three mutually exclusive but exhaustive groups:
- Medical Only
- Indemnity
- Denied
Samples of the medical only and indemnity claim are drawn based on the number of claims at the location. In smaller locations, all denied claims are reviewed. For larger locations, sampling is used, but the samples are larger relative to the population than for medical-only and indemnity claims. In addition, any claims at that location for which a complaint was received are reviewed. In a new practice, the AU abbreviates the audit if the rate of violations is very low in the first part of the audit.
An audit of a location can take from two to six weeks to complete. An auditor reviews each file for approximately 120 violations that are grouped for the purposes of the Annual Report into 21 groups. These range from minor violation such as errors on the claim log submitted to the AU or mistakes in the benefit notice process to serious violations such as unsubstantiated denials of compensability.
Half of all citations are issued for failures related to the Benefit Notice process. These usually represent minor violations. They are also an indicator that the Benefit Notice process has become unnecessarily complex. A streamlining of this process would reduce violations while improving the understanding of injured workers.
Issues:
1. Current data reporting by the Audit Unit cannot be used to evaluate the system’s overall performance.
As currently reported, the data in the annual report cannot be used to evaluate system performance. The most serious problem is that the mix of targeted and random audits changes from year to year. Targeted locations are obviously likely to have more frequent violations and more serious violations. The age of claims reviewed has changed since auditing started. The number of claims reviewed, the percent of all claims reviewed, the total indemnity paid on claims, and the average indemnity/claim have also changed.
Because the data are not reported in sufficient detail, these differences make it impossible to evaluate the system for a particular year or changes in the system over time.
Solution:
Two possible solutions are available. Either the AU could develop data analysis methods for reporting key benchmarking data on the system or the AU could make the data available in such a way as to allow outside parties to perform their own evaluations.
For example, two important system-monitoring benchmarks are:
- Timeliness of payment of compensation
- Amount of unpaid compensation
These cannot be assessed from the current reporting. However, these issues could be assessed if the AU made available data for each audited location giving:
1. Whether the audit is random or targeted audit
2. Selection weight if a random audit
3. The following data on each location and the system
DATA REPORTING |
Medical Only |
Indemnity |
Denied |
| Number of claims at location By year of injury | |||
| Number of claims audited at location By year of injury | |||
| Number of claims system wide By year of injury |
4. Violation data at each location would be reported by type of claim (medical only, indemnity, denied) and year of injury.
These data are already collected but not published by the Audit Unit.
Statistical methods would be developed to standardize the reporting across the system and across years, correcting for differences in sampling and for the size of the locations sampled. This methodology could be constructed so that reporting on each benchmark would reliably reflect the system’s performance.
Development of such a system for implementation by the AU would require approximately two months of work by an analyst and four meetings with the AU and stakeholders to define the appropriate benchmarks and to assess the sampling methods used in each of the previous several years.
2. The auditing and penalty assessment program of the Division of Workers’ Compensation/Audits Unit does not accomplish the goal of encouraging better performance by claims administrators.
The current penalty structure is poorly designed. It will not effectively motivate improved performance by poor locations. At the same time, it unnecessarily fines good performers.
Some problems:
A. Penalties as currently structured are unlikely to be an effective incentive for encouraging insurers to comply with regulations.
- Compliance officers audited 12,400 cases in 1996 or approximately 0.5% of the universe of cases.
- To a first approximation, the chance of getting ‘caught’ for any violation is 200-1. Unless the penalties exceed 200 times the payment avoided, the insurer would still have a financial incentive to underpay or avoid payment.
- As an example, penalties assessed for unpaid compensation were $200,000 on claims with $480,000 in unpaid compensation in 1996. A ratio of 0.4 - 1 rather than 200 - 1.
- While penalties were $200,000, unpaid compensation, as currently defined in the system, likely ran to tens of millions of dollars.
B. While larger locations will have somewhat more files audited, these locations will still face lower penalties relative to the number of total violations or the amount of unpaid compensation. This is true because any claim is less likely to be audited at a larger location.
C. We should not have "zero tolerance" for mistakes. To expect perfection is to expect inefficiently high levels of oversight by insurers. Consequently, insurers should be given reasonable targets for performance and only penalized for failure to meet those goals.
Solution:
When the Audit Unit was originally set-up, the Division wisely chose a strategy that randomized location selection and relied on sampling. However, the Division has never taken full advantage of the power of this technique to improve system performance and discourage bad practice. The Commission should undertake a review of the Audit penalty assessment mechanisms.
One advantage of doing random sampling is that from a random sample we can infer something about the larger underlying population. By taking a random sample of cases from a location’s total population of cases, we expect to be able to project their typical action on cases. In this respect, it is correct to extract a relatively small sample of cases even from locations with large caseloads. The next step is to use this information to apply penalties to the whole population of cases.
DWC should not expect perfect compliance with regulations. Compliance is expensive, and at some point ensuring of that every "i" is dotted and "t" is crossed is prohibitive. However, the current level of error seems unacceptably high. As an alternative to applying a penalty to each infraction, a different approach would be to apply penalties to levels of infraction that exceed some specified level.
Here is a brief outline of one alternate penalty structure:
- The current rate of each violation is estimated for the system. For example, among audited claims in 1996, approximately 13% of indemnity claims had outstanding unpaid compensation. This is consistent with previous year’s results. We will assume this is accurate for this example.
- Stakeholders and policymakers would estimate a reasonable rate of mistakes for each type of violation. For example, consensus may be that a 3% mistake rate at some average dollar figure is acceptable.
- Each year, the system would target improvements in the accepted level of violations, until the goal is reached. For example, year 1, 11%; year 2, 9%, year 3, 7%; year 4, 5%; year 5 and later, 3%.
- Penalties would be assessed for performance of locations against this goal, rather than on individual violations.
- Locations beating the benchmarks would avoid penalties, while those that missed the mark would be subject to penalties that would be progressively harsher the further the location missed the benchmarks. For example, locations meeting or beating the target percent would face no penalties, even though they were out of compliance on some claims. For each 2% above the target, a location might face a doubling of the penalty rate.
- Penalties estimated on the sample would be applied to the whole population of claims at that location. This would make the incentive to meet benchmarks much stronger. For example, if 5% of claims were audited at the location, the number of infractions would be estimated at 20 times those found. This balances the fines faced by small and large locations.
- Penalty structures would be tested to determine the level of fines that would have been applied using historical data. Different penalty structures could then be evaluated for cost and impact on incentives of the worst performers.
This sampling and penalty structure is only one of many that could be developed. Many issues need to be considered such as legal restrictions, statistical reliability, revenue neutrality, avoiding too harsh or too soft penalties, etc.
Conclusion:
It is quite easy to develop the data necessary to evaluate the system’s performance. The AU collects these data and simply needs to analyze it effectively or make the data available to outside evaluators.
Developing better penalty structures is a fairly complex issue that would require assessment of several approaches and estimates of the costs to insurers based on the historical record. All stakeholders should be involved in the development of the performance targets and evaluation of appropriate penalty structures. This process would likely involve a series of meetings with the stakeholders combined with work by a technical team to develop alternatives, estimate the impact of the alternatives, refine the proposals, and develop statutory or regulatory language for implementation.
Activities of the Audit Unit
1993 |
1994 |
1995 |
1996 |
1997 |
|
| Number of Audits | 61 |
56 |
64 |
55 |
39 |
| Self-Insured | 15 |
10 |
11 |
15 |
15 |
| TPA | 18 |
15 |
22 |
22 |
13 |
| Insured | 28 |
31 |
31 |
18 |
11 |
| Random | 55 |
49 |
54 |
48 |
29 |
| Non-Random | 6 |
7 |
7 |
7 |
10 |
| Claim Files Reviewed in Audits | 14,316 |
13,196 |
16,261 |
12,436 |
8,504 |
| Medical-only claim files | 5,692 |
4,876 |
6,047 |
4,901 |
3,260 |
| Other claim files | 8,624 |
8,320 |
10,214 |
7,535 |
5,244 |
| Investigations | |||||
| Number of Investigations | 20 |
22 |
40 |
35 |
18 |
| Number of Claims Files Reviewed | 223 |
54 |
116 |
98 |
89 |
Discussion of Current Audit Targeting Process
Our analyses of complaint data, both the geographical bias and source of complainant bias suggested that targeting is being done inefficiently.
The following charts suggest that these earlier analyses were correct. We compared the total number of violations and the total penalty dollars to the number of indemnity and denied files audited in each region. Several things are clear from the data.
- The number of violations per file was higher in Southern California.
- The penalties assessed per file were higher in Southern California
- In two of the three years, the violations per file on the targeted audits in Northern California were higher than the violations per file on random audits in southern California.
However:
- Nearly 60% of the targeted audits are done in Northern California.
- The ratio of targeted/random audits is 50% higher in Northern California.
This suggests a serious failure in the targeting process. Randomly selecting Southern California locations would be nearly as good and often better at detecting violations as the current targeting of Northern California locations.
These data indicate that the targeting process is not being performed very effectively. Consequently, review of targeting procedures would be in order, especially if targeted audits were to be expanded as percent of all audits.
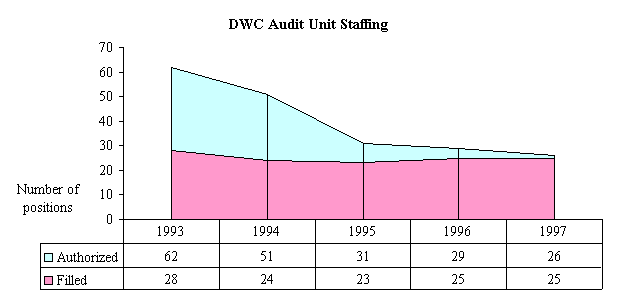
Discussion of the Recommendation to Eliminate Administrative Penalties at the PAR Level
The research team spent considerable time analyzing and discussing the recommendation to eliminate administrative penalties at the PAR level and for most violations at locations that pass the FCA. This review was triggered in part by comments at the Advisory Committee and written comments submitted to the Commission. After a thorough review we recommend this approach for the following reasons:
- The main purpose of the administrative penalties is to motivate claims administrators to improve performance or maintain already good performance. The incentive related to penalties is a product of the size of the penalty and the probability of that penalty being applied. Increasing the penalty amounts increases the incentive without substantially increasing the cost of the audit process. Increasing frequency of application of penalties directly increases the cost of auditing to the Audit Unit and ultimately employers.
- Since Audit Unit resources are necessarily finite and it is time consuming and resource intensive to document each violation sufficiently to apply penalties, it would be difficult to dedicate sufficient resources to apply fines to all violations in all instances and still accomplish the goal or auditing all locations at least once every five years.
- The "optimal" level of violations is not zero. To be perfect, locations would have to expend excessive resources. Some mistakes even in excellent operations are expected. In fact, auditors often find that locations overpay compensation. Requiring locations to be too good would raise the cost of claims administration and, in turn, the cost of compensation insurance.
- Employers and workers ultimately pay the cost of compensation insurance including administration and expected penalties. Employers pay in higher costs and workers pay in lower wages. An audit function should efficiently accomplish the task of monitoring and improving performance without creating excessive costs.
- As part of the focus on the worst performers and an effort to improve and fairly apply penalties, the Research Team is recommending substantial increases in penalties on the worst performers. It was felt that these increases should be balanced by reductions in the administratively expensive and mostly ineffective application of numerous but small penalties on adequate performers.
Consequently, the proposed process accomplishes a higher degree of incentive to improve performance while reducing the cost of the average audit. Penalties on the whole are expected to remain approximately at current levels, but the impact will be substantially increased.
PAR and FCA Performance Standards
The PAR audit is meant to be a screening process to eliminate the need for a resource intensive audit of locations that perform at acceptable standards. The FCA process is meant to determine which locations have performance levels that justify application of the administrative penalties at the level recommended in the Report.
To accomplish these goals, the criteria for passing or failing the PAR process should:
- Accurately identify all or nearly all of the worst performing locations for examination at the FCA level, while
- Not subjecting more than a few locations with adequate performance to the additional demands of an FCA level review, and
- Do this in a way that is clear to participants, and
- Flexible enough to be adjusted to changes in performance and community standards.
Similarly the criteria for passing or failing the FCA process need to accurately identify the worst performing locations for application of substantial penalties, while not subjecting adequately performing locations to unwarranted penalties. Again, these standards should be clear to participants and allow flexibility to respond to changing conditions.
Development of PAR Performance Standards
At the PAR level, the performance standards are limited to the six Key Indicators developed for review at this stage. Two specific sets of questions required treatment in the development of the PAR Performance Standards:
- Could these six Key Indicators accurately identify the worst performers?
- What is the best way to construct the performance standard?
In essence, these questions are complementary. At least the standard should identify the worst performers and move them to the FCA and adequate performers should not be incorrectly selected for the FCA. However, the "best" method would accomplish these goals and be easily understood and establish clear and comparable measures of performance among locations.
Two Methods Compared
A number of approaches were tested that fall into two basic categories:
- A performance standard is established for each Key Indicator. Failure on one or more of the individual standards would result in failure at the PAR level.
- A composite score, combining all of the Key Indicators in a single measure, could be developed. A Standard for the composite score could be established, and the failure to achieve the combined score would result in failure at the PAR level.
The Research Team recommends the composite score method for the following reasons:
- The composite score approach captures those locations that performed poorly across the board but may have been just good enough to avoid failing on any (or enough) Key Indicators to fail at the PAR level.
- The nature of any sampling process is the possibility of drawing an unrepresentative sample in any individual trial. This problem is particularly acute if the sample is subject to several tests, any of which would result in failure. This problem is substantially reduced if a composite score is used instead. Adequate locations will be less likely to be failed and poor performing locations will be less likely to pass.
- Composite measures make it easier to place extra emphasis on indicators that the community feels are more important. That is, weights can be attached to each individual Key Indicator measure which, when combined, improve the overall measure of performance. This is more difficult and less effective when individual pass/fail levels are set for each Indicator.
- Finally, in testing both approaches against past audit performance, the composite score proved more effective at both identifying the worst performers and not incorrectly failing adequate performers.
Testing the two methods
Each approach was tested against combined Audit Data from 1995 and 1996. Separately, the approaches were tested against 1997 audit data after the best approach in each method was determined.
Two methods were used to select and rank the worst performers from these earlier audits. First, the Audit Unit had selected which locations would have been subject to an expanded audit based on their performance against criteria for 1) unpaid compensation, 2) benefit notice requirements, and 3) unsupported denials. Second, the Audit Unit was asked to independently rank the poorest performing locations from 1995 and 1996.
Each of the two approaches was tested against these data and the best approach was refined against its ability to select the poorest performers while avoiding selection of adequate performers. The best of the composite scoring approaches was substantially superior to the best of the methods based on passing or failing on individual criteria. The recommended approach selected all locations that failed on 2 or more of the Audit Unit’s three tests. In addition, the recommended method selected 19 locations for FCA including 19 of the 20 locations selected as the worst performing locations by the Audit Unit while missing only the 15th ranked location.
Recommended Method
The recommended method is as follows:
- A measure is calculated for each Key Indicator.
- The recommended composite measure is created by weighting the unsupported denial measure by three.
- Finally, a Performance Standard is selected against which locations will be compared.
For unsupported denials, this is the percent of violations in the sample of denied cases, but no score is give if the number of violations is less than two.
For the other key indicators, except unpaid compensation, the measure is the number of violations divided by the number of files with exposure for that violation. For example, indemnity claims with salary continuation instead of TTD would not be counted in the denominator for the Late 1st Payment of TTD Indicator.
For unpaid compensation the measure takes into account of both the frequency and amount of unpaid compensation simultaneously. First an historical average for unpaid compensation on files with exposure for indemnity payments is calculated for all audited indemnity files. Each location then has a Multiplier calculated which is
(Average Unpaid Compensation at the Location) / (Historical Average Unpaid Compensation)
The measure is then calculated as:
(Number of violations for Compensation Due) / (Number of files with exposure) * Multiplier
This increases the importance of unsupported denials that are considered critical but relatively rare events. The VR notification measure is weighted by 0.3. This reflects the high rates of violation found, but relatively few files have exposure for this violation. The unpaid compensation is in effect already weighted by the impact of the multiplier on the frequency of violations.
A composite score for the location that exceeds the Performance Standard, reflecting poor performance, would subject the location to the Full Compliance Audit. The Research Team recommends a Performance Standard set at the 15th percentile. That is, the worst 15% of locations, based on historical performance levels, would be subjected to a FCA. Periodically, the Performance Standard can be adjusted based on additional audit data, changes in community attitudes towards adequate performance, and/or Audit Unit resources.
An additional benefit has been attributed to the composite approach. A number of participants commented on the attractiveness of a measure that allows comparison of the performance of different claims administrators. This would increase incentives to perform well and increase employers’ knowledge of claims practices when selecting a compensation insurer or third party administrator.
FCA Performance Standards
The FCA Performance Standard mirrors the PAR Performance Standard except that the number of criteria involved in the composite score is expanded to include all administrative violations and not just the six Key Indicators. For example, instead of using only the total compensation due as a measure, the sum of each violation would be used (overpayments and underpayments would not cancel) and late payment and failure to pay SII would also be included.
The standard for performance on the FCA will reflect the expectation that approximately � of the locations undergoing the FCA will be subject to administrative penalties, representing the worst 5% to 10% of claims administrators.
Proposed Administrative Penalty Structure
Summary
After consultation with the Audit Advisory Committee and discussions with the Commissioners and stakeholders, the Research Team is proposing to structure penalties for violations according to a stepped formula that matches the size of the penalty to the size of the location audited.
This format retains the qualities of
- Fairly distributing the impact of penalties across all locations,
- Improving the incentives for good performance,
- Without requiring the complicated statistical adjustments associated with extrapolation.
Penalties result after a two-stage evaluation. First, a location has to fail the PAR audit process. Second, the location has to fail the Full Compliance Audit (FCA). We propose a set of criteria for determining failure at each stage. Under extraordinary circumstances a location may be targeted for a non-random Full Compliance Audit.
Penalty amounts applied to any individual violation at locations failing the FCA are calculated as a multiple of current penalty amounts based on the rank of the location by size relative to all other locations. Size is measured by the number of indemnity files that were in the population subject to selection for audit. The relative sizes of locations are also adjusted to reflect the size of the samples drawn. This is an important step because the location is subject violations found in the sample.
Using criteria for passing/failing the two stage process, PAR and FCA, and penalties adjusted to make them equitable for all locations, we reviewed the impact on 1995 and 1996 results of penalties that would have been applied under the recommended formula. We evaluated several penalty structures. One proposal applied current penalty levels to the locations in the smallest size rank and adjusted upward for the rank of each larger location. A second proposal set the current penalty level at the median size location and adjusted the penalties for smaller locations down and larger locations up.
A third proposal was evaluated that represented a compromise between these two approaches. This method compresses the variation in penalty amounts between the smallest and largest locations. This approach avoids reducing penalties below current levels without raising penalties on the largest locations beyond what the Advisory Committee felt were acceptable levels.
Penalty Structure
Current administrative penalties for audit violations are inequitable applied to locations of different size. Consequently, incentives for good performance are poorly aligned with the penalties for locations that handle the vast majority of claims. The smallest locations, which handle a small fraction of claims face economic consequences that are twenty-five to fifty times as severe as those faced by the larger locations that handle eighty percent of claims.
The research team at the August meeting of the Audit Advisory Committee proposed two methods for improving both the equity of the penalty structure and the incentives for good performance that the penalties are meant to encourage:
Method "A" proposed extrapolating the number of violations detected in the sample to the population of claims at the location using sophisticated, but complicated statistical estimation techniques similar to those used by the Federal government welfare and Medicare audits.
Method "B" proposed a simpler method that only required adjusting the size of the administrative penalty to the size of the location.
In discussions with the Advisory Committee, Commissioners, and the compensation community were all in favor of the simpler Method "B." This method is applied as follows.
- All locations reporting claims for the Annual Inventory of Claims conducted by the Audit Unit are ranked into ten groups based on the size from the smallest 10% of locations to the largest 10% of locations. Each location’s size is based on the number of indemnity files that could be subject to audit for that particular audit year. Indemnity files were chosen as the basis because nearly all violations are applied to these files, and some locations handle only indemnity files while others handle medical only and indemnity. This process ranks size most effectively and fairly according to exposure for violations.
- Each location is then assigned administrative penalty amounts for each violation based on the location’s size.
- If a location ultimately fails the FCA, the administrative penalties for each violation are calculated based on these proposed penalties amounts.
- Size ranks and the penalty amounts for each violation type applicable to the current year’s audits would be based on the previous year’s Annual Inventory of Claims. These ranks and penalties would be published each year by the DWC.
The following table lists the approximate size of each rank of locations and the accompanying proposed penalties.
Tables 1-A and 1-B on the following page show other proposed approaches that were considered.
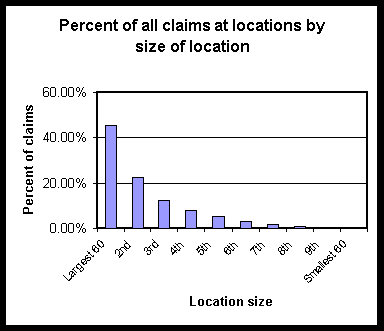
Proposed Administrative Penalties
These penalties were applied to audits from 1995 and 1996. Total penalty amounts for the recommended penalty structure were approximately equal to current penalty amounts. Fewer locations would have been subject to penalties. This reflects the two-stage, PAR and FCA, process where only the worst performers are subject to penalties. However, penalties would have been substantially larger for those locations that would have failed the FCA based on proposed Performance Standards.
The following two alternatives for administrative penalties were also reviewed by the Research Team.
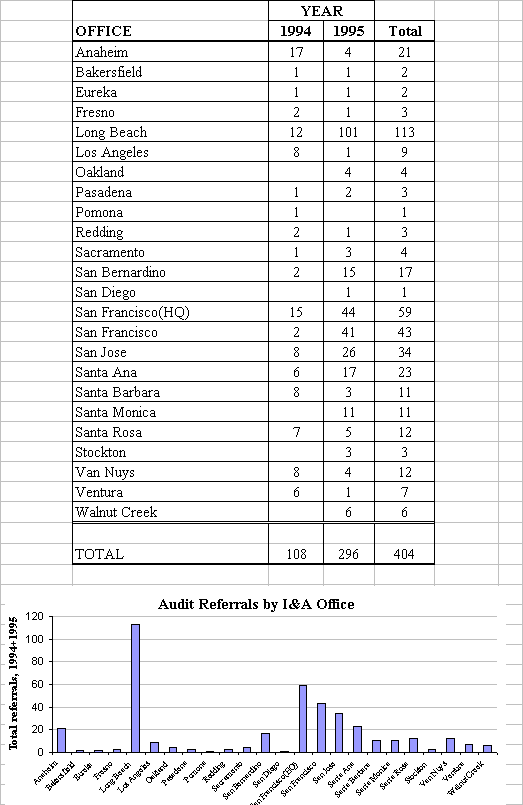
Impact of Single Rate Payments
Summary
The current statutes set different weekly rates, minimums and maximums for Temporary Disability (TD), Permanent Disability (PD) and Vocational Rehabilitation Maintenance Allowance (VRMA). Even within PD, there are changing maximum payment levels. These changing rates are confusing to injured workers and make payment calculations more difficult and prone to error for insurers.
The Audit Advisory Committee and the Commission Research Team agreed that a single rate of compensation for all indemnity benefits was desirable. This rate would be set at the current Temporary Total Disability rate. The amount paid of any species would not change, only the rate at which it is paid out. PD total amounts would be determined according to the current schedule, but paid out at the TTD. For VRMA, the $16,000 cap would still be in place, but VRMA would be paid at the higher rate, and the worker allowed to supplement the cap rather than the weekly payment.
However, for insurers and self-insured employers changing the rate of payment, even if the total amount remains the same, has an implication for cash flow and interest earnings on reserves. Since interest earnings are an important source of income for insurers and employers, the Advisory Committee asked the research team to estimate the impact of this change.
The Commission Research Team undertook this evaluation using a transaction dataset supplied by the California Workers’ Compensation Institute (CWCI). The Research Team determined that the impact would reduce insurer/employer earnings from interest income on PPD reserves by 4.9% and on VRMA by 2.5%. This is equal to between 0.2% and 0.4% of all benefit payments.
The table on the following page summarizes these findings.
Interest Rate |
|||
7% |
11% |
15% |
|
| Interest Earnings as Percent of Indemnity Payments | |||
| TTD: interest earned | |||
| Current rate | 4.4% |
6.9% |
9.4% |
| Single rate | Same |
Same |
Same |
Change as percent of TTD indemnity payments |
0.0% |
0.0% |
0.0% |
| PPD: interest earned | |||
| Current rate | 12.9% |
20.2% |
27.6% |
| Single rate | 12.3% |
19.3% |
26.3% |
Change as percent of all PPD indemnity payments |
-0.62% |
-0.97% |
-1.32% |
| VRMA: interest earned | |||
| Current rate | 11.4% |
17.9% |
24.5% |
| Single rate | 11.1% |
17.5% |
23.9% |
Change as percent of all VRMA indemnity payments |
-0.28% |
-0.45% |
-0.61% |
| Change as percent of all Indemnity Payments | -0.34% |
-0.57% |
-0.73% |
| Change as percent of all benefit payments (medical+indemnity) |
-0.20% |
-0.32% |
-0.42% |
Methodology:
Estimating interest earnings under current benefit rates
With the assistance of CWCI, the Research Team drew a sample of 70,000 claims from the ICIS Database developed by the Institute. The claims covered resolved claims with dates of injury in 1993 and 1994. The dataset is a subset of the ICIS data and includes all indemnity payments, date of payment, amount paid, type (TTD, PPD, etc.), date of injury, and average weekly wage. From these data, we reconstructed the indemnity payments and the timing of these payments for a representative sample of indemnity claims.
Once this stream of payments was constructed, we were able to calculate the interest earnings on incurred but not paid indemnity. For each payment the number of days from date of injury to payment date was calculated. Then given the payment amount and a particular interest rate, the interest was calculated for the earnings from date of injury to payment date.
(Days from DOI to payment date) * (Paid amount) * (Daily interest rate) = Interest earned
The sum of these interest earnings over the life of the claim was calculated for each species of benefit.
Reestimating interest earnings under a single rate set at the TTD weekly rate
First, the original weekly rate under which each benefit was paid was calculated for each case using the average weekly wage and the appropriate minimum/maximum for the date of injury. The TTD rate and the VRMA rate can be calculated in this manner. Given the limitations on the data, the PPD weekly rate can only be estimated since we do not have the final rating. For this reason, the weekly rate was assumed to be $140 for all PPD payments. This will be slightly high for very low wage earners with minor low ratings, and slightly low for the small number of moderate to high wage earners with very high ratings.
Since the original payments often represent multiple or partial weeks or other modifications, each paid amount was converted to a multiple or fraction of weeks paid for that payment date. For example: if a worker receiving VRMA at $246/week receives a last payment of $423. This is calculated to represent $423/$246 = 1.71 weeks.
The object of this effort was to determine the impact of speeding up the payment of benefits without changing the total amount paid for any species of indemnity. Therefore, the sum all payments for each species was calculated for each case, this is referred to as the "pool." This was the total amount that would be paid under the higher single rate.
Then, each payment in the original data set was recalculate using the TTD rate estimated for each case. This formula was:
NewPaid_amount = (TTD rate) * (multiple/fraction of weeks paid)
These payments were continued until the "pool" was exhausted.
In addition, because in many, if not most, cases PPD payments are concluded by a lump sum payment at the time of settlement, the amount paid out in periodic payments for PPD was calculated as the "pool" minus the Final Payment. This amount was paid out until exhausted, and then the Final Payment was made in the same amount and on the same date as the original dataset.
Interest earnings were calculated again using this alternate stream of payments and the same formula as for the original stream. For TTD benefits, these earnings were the same since the benefit rate was the same. For PPD and VRMA, interest earnings were less representing the impact of accelerating the rate of payment when switching from the current lower rates to the TTD rate for PPD and VRMA payments.
For purposes of estimating the change in interest earnings as a percent of indemnity benefits and for all benefits, the following factors were used:
Fraction |
Source |
|
| TTD as percent of all indemnity | 31.1% |
ICIS |
| PPD as percent of all indemnity | 51.5% |
ICIS |
| VRMA as percent of all indemnity | 7.7% |
ICIS |
| Indemnity as percent of all benefits payments | 57.0% |
WCIRB Annual Report 1998 |
Finally, different interest rates were used representing 7%, 11%, and 15%. Greg Vach suggested 11% as consistent with self-insured employers’ internal rate of return on reserved funds. 7% was selected to represent insurer earnings under more restrictive regulations concerning reserves. 15% was selected as a high-end estimate. The impact under other interest rates can be estimated at the request of the Audit Advisory Committee.
Proposed Legislation
COMMISSION ON HEALTH AND SAFETY AND WORKERS' COMPENSATION
MEMORANDUM
Date: December 1, 1998
To: Christine Baker, Executive Officer
From: C. L. Swezey, Consultant
Re: Proposed Legislation to Amend Labor Code §§62.5, 75, 78, 129, 129.5. and 4628
There follow proposed amendments to §§62.5, 75, 78, 129, 129.5. and 4628 to implement the recommendations in the CHSWC Report on the DWC Audit Function prepared after review by the project team on November 30, 1998. The proposed changes would:
(1) Abolish the Workplace Health and Safety Revolving Fund and provide for the deposit of audit and §4628 penalties in the Workers' Compensation Administration Revolving Fund and funding CHSWC from the latter fund.
(2) Require profile audit reviews of each audit location every five years in addition to targeted audits.
(3) Require full compliance audits of each audit unit that fails to meet a profile audit review performance standard.
(4) Require a repeat audit within two years for audit subjects that fail a full compliance audit.
(5) Require notices of compensation due whenever discovered in an audit or profile audit review regardless of whether the audit subject meets the performance standards.
(6) Relieve from penalties any audit subject that meets or exceeds the profile audit review standard.
(7) Relieve from penalties, except for nonpayment or late payment of compensation, any audit subject that meets or exceeds the full compliance audit performance standards.
(8) Provide for a full compliance audit failure penalty schedule that adjusts penalty levels relative to the size of the audit location to mitigate inequality between total penalties assessed against small and large audit subjects.
(9) Require the administrative director to adopt a profile audit review standard, full compliance audit performance standards, target audit criteria, and a full compliance audit failure penalty schedule that adjusts penalty levels relative to the size of the audit location to mitigate inequality between total penalties assessed against small and large audit subjects and to annually publish and make available to the public on request a list ranking all insurers, self-insured employers, and third-party administrators audited according to their performance..
(10) Make the basis for the $100,000 penalty consistent with basis for penalties fixed by the Insurance Commissioner pursuant to Insurance Code §790.035.
(11) Create a presumption that any employer, insurer, or third party administrator that fails to meet the full compliance audit performance standards in two consecutive full compliance audits is presumed to have engaged in a general business practice of discharging and administering its compensation obligations in a manner causing injury to those dealing with it.
(12) Provide for WCAB review of penalties assessed by the administrative director under §129.5(d).
(13) Provide for audits of the adjustment of claims against the Uninsured Employers Fund by the claims and collections unit of the Division of Workers' Compensation.
PROPOSED BILL:
[Matter to be deleted is typed in strike through. Matter to be added is in typed in italics. Subsections which require no change have not been retyped, only the first few words are shown with the notation [No change].]
SECTION 1. Section 75 of the Labor Code is amended to read:
§75 (a) There is in the [No change].
(b) The commission shall [No change].
(c) The initial terms [No change].
(d) The commission shall meet every other month and upon call of the chair. Meetings shall be open to the public. Members of the commission shall receive one hundred dollars ($100) for each day of their actual attendance at meetings of the commission and other official business of the commission and shall also receive their actual and necessary traveling expenses incurred in the performance of their duty as a member. Payment of per diem and traveling expenses may be made from the Workplace Health and Safety Workers' Compensation Administration Revolving Fund, when appropriated by the Legislature.
SECTION 2. Section 78 of the Labor Code is amended to read:
§78 (a) The commission shall [No change].
(b) Civil and administrative penalties assessed pursuant to Sections 129.5 and 4628 shall be deposited in the Workplace Health and Safety Revolving Fund, which is hereby created in the state treasury Workers' Compensation Administration Revolving Fund. Proceeds of the fund Moneys from the Workers' Compensation Administration Revolving Fund, when appropriated by the Legislature, shall be expended by the department, upon approval by the commission, for funding the grants under subdivision (a), and by the commission for payment of the commission's expenses incurred under this chapter.
[In the event that §62.5 is not in effect or does not provide for a Workers' Compensation Administration Revolving Fund when the proposed bill becomes effective, the following SECTION 2.5 must be included:]
SECTION 2.5. Section 62.5 is added to the Labor Code to read:
§62.5 (a) The Workers' Compensation Administration Revolving Fund is hereby created as a special account in the State Treasury. Proceeds of this fund may be expended by the department, upon appropriation of the Legislature, for the administration of the workers' compensation program as set forth in this division and Division 4 (commencing with §3200) other than the activities financed pursuant to Section 3702.5, and, upon approval of the Commission on Health and Safety and Workers' Compensation for funding grants under Section 78 and by that commission for payment of the commission's expenses incurred under Chapter 3 of this division, and shall not be used for any other purpose.
(b) The fund shall consist of money from the General Fund appropriated for those purposes and from civil and administrative penalties assessed pursuant to Sections 129.5 and 4628.
SECTION 3 Section 129 of the Labor Code is amended to read:
§129 (a) To make certain that injured workers, and their dependents in the event of their death, receive promptly and accurately the full measure of compensation to which they are entitled, the administrative director shall audit insurers, self-insured employers, and third party administrators to determine if they have met their obligations under this code. Each audit subject shall be audited at least once every five years. At least half of the The audit subjects shall be selected and the audits conducted at random, and the remaining subjects shall be selected pursuant to subdivision (b). The results of audits of insurers shall be provided to the Insurance Commissioner and the results of audits of self-insurers and third party administrators shall be provided to the Director of Industrial Relations. Nothing in this section shall restrict the authority of the Director of Industrial Relations or the Insurance Commissioner to audit their licensees.
(b) The administrative director shall establish priorities for audits based on information obtained from the Benefit Notice program established under Section 138.4, through information and assistance services and other factual information that indicates an insurer, self-insured employer, or third party administrator is failing to meet its obligations under this division or Division 4 (commencing with Section 3200) or the regulations of the administrative director. schedule and conduct audits as follows:
(1) A profile audit review of every audit subject shall be conducted once every five years and on additional occasions indicated by target audit criteria. The administrative director shall annually establish a profile audit review performance standard that will identify the poorest performing audit subjects.
(2) A full compliance audit shall be conducted of each profile audited subject failing to meet or exceed the profile audit review performance standard. The full compliance audit shall be a comprehensive and detailed evaluation of the audit subject's performance. The administrative director shall annually establish a full compliance audit performance standard that will identify the audit subjects that are performing satisfactorily. Any full compliance audit subject that fails to meet or exceed the full compliance audit performance standard shall be audited again within two years.
(3) A targeted profile audit review or a full compliance audit may be conducted at any time in accordance with target audit criteria adopted by the administrative director. The target audit criteria shall be based on information obtained from benefit notices, from information and assistance officers, and other reliable sources providing factual information that indicates an insurer, self-insured employer, or third party administrator is failing to meet its obligations under this division or Division 4 (commencing with Section 3200) or the regulations of the administrative director.
(c) If, as a result of an a profile audit review or a full compliance audit, the administrative director determines that any compensation, interest, or penalty is due and unpaid to an employee or dependent, the administrative director shall issue and cause to be served upon the insurer, self-insured employer, or third-party administrator a notice of assessment detailing the amounts due and unpaid in each case, and shall order the amounts paid to the person entitled thereto. The notice of assessment shall be served personally or by registered mail in accordance with subdivision (c) of Section 11505 of the Government Code. A copy of the notice of assessment shall also be sent to the affected employee or dependent.
If the amounts are not paid within 30 days after service of the notice of assessment, the employer shall also be liable for reasonable attorney's fees necessarily incurred by the employee or dependent to obtain amounts due. The administrative director shall advise each employee or dependent still owed compensation after this 30-day period of his or her rights with respect to the commencement of proceedings to collect the compensation owed. Amounts unpaid because the person entitled thereto cannot be located shall be paid to the Workplace Health and Safety Revolving Fund Workers' Compensation Administration Revolving Fund. The Director of Industrial Relations shall promulgate rules and regulations establishing standards and procedures for the payment of compensation from moneys deposited in the Workplace Health and Safety Revolving Fund Workers' Compensation Administration Revolving Fund whenever the person entitled thereto applies for compensation.
(d) A determination by [No change].
(e) Annually, commencing on April 1, 1991, the administrative director shall publish a report detailing the results of audits conducted pursuant to this section during the preceding calendar year. The report shall include the name of each insurer, self-insured employer, and third-party administrator audited during that period. For each insurer, self-insured employer, and third-party administrator audited the report shall specify the total number of files audited, the number of violations found by type and amount of compensation, interest and penalties payable, and the amount collected for each violation. The administrative director shall also publish and make available to the public on request a list ranking all insurers, self-insured employers, and third-party administrators audited during the period according to their performance measured by the profile audit review and full compliance audit performance standards.
These reports shall not identify the particular claim file which that resulted in a particular violation or penalty. Except as required by this subdivision or other provisions of law, the contents of individual claim files and auditor's working papers shall be confidential. Disclosure of claim information to the administrative director pursuant to an audit shall not waive the provisions of the Evidence Code relating to privilege.
(f) A profile audit review of the adjustment of claims against the Uninsured Employers Fund by the claims and collections unit of the Division of Workers' Compensation shall be conducted at least every five years. The results of this profile audit review shall be included in the report required by subdivision (e).
SECTION 5. Section 129.5 of the Labor Code is amended to read:
§129.5 (a) The administrative director shall may assess an administrative penalty against an insurer, self-insured employer, or third-party administrator for any of the following:
(1) Failure to comply with the notice of assessment issued pursuant to subdivision (c) of Section 129 within 15 days of receipt.
(2) Failure to pay when due the undisputed portion of an indemnity payment, the reasonable cost of medical treatment of an injured worker, or a charge or cost implementing an approved vocational rehabilitation plan.
(3) Failure to comply with any rule or regulation of the administrative director.
(b) The administrative director shall promulgate regulations establishing a schedule of violations and the amount of the administrative penalty to be imposed for each type of violation. The schedule shall provide for imposition of a penalty of up to one hundred dollars ($100) for each violation of the less serious type and for imposition of penalties in progressively higher amounts for the most serious types of violations to be set at up to five thousand dollars ($5,000) per violation. The administrative director is authorized to impose penalties pursuant to rules and regulations which give due consideration to the appropriateness of the penalty with respect to the following factors:
(1) The gravity of the violation.
(2) The good faith of the insurer, self-insured employer, or third-party administrator
(3) The history of previous violations, if any.
(4) Whether the audit subject has met or exceeded the profile audit review performance standard.
(5) Whether a full compliance audit subject has met or exceeded the full compliance audit performance standard.
(6) The size of the audit subject location.
(c) The administrative director shall assess penalties as follows:
(1) If after a profile audit review the administrative director determines that the profile audited subject met or exceeded the profile audit review performance standard, no penalties shall be assessed, but the audit subject shall be required to pay any compensation due and penalties due under subdivision (d) of Section 4650 as provided in subdivision (c) of Section 129.
(2) If after a full compliance audit the administrative director determines that the audited subject met or exceeded the full compliance audit performance standards, penalties for unpaid or late paid compensation, but no other penalties, shall be assessed. The audit subject shall be required to pay any compensation due and penalties due under subdivision (d) of Section 4650 as provided in subdivision (c) of Section 129.
(3) If after a full compliance audit the administrative director determines that the audited subject failed to meet the full compliance audit performance standards, penalties shall be assessed as provided in a full compliance audit failure penalty schedule to be adopted by the administrative director. The full compliance audit failure penalty schedule shall adjust penalty levels relative to the size of the audit location to mitigate inequality between total penalties assessed against small and large audit subjects. The penalty amounts provided in the full compliance audit failure penalty schedule for the most serious type of violations shall not be limited by subdivision (b), but in no event shall the penalty for a single violation exceed forty thousand dollars ($40,000).
(c) (d) The notice of [No other change].
(d) (e) In addition to the penalty assessment permitted by subdivisions (a), (b) and (c), the administrative director may assess a civil penalty, not to exceed one hundred thousand dollars ($100,000), upon finding, after hearing, that an employer, insurer, or third party administrator for an employer has knowingly committed and or performed with such frequency as to indicate a general business practice any of the following:
(1) Induced employees to accept less than compensation due, or made it necessary for employees to resort to proceedings against the employer to secure compensation.
(2) Refused to comply with known and legally indisputable compensation obligations.
(3) Discharged or administered compensation obligations in a dishonest manner.
(4) Discharged or administered compensation obligations in a manner as to cause injury to the public or those dealing with the employer or insurer.
Any employer, insurer, or third party administrator that fails to meet the full compliance audit performance standards in two consecutive full compliance audits shall be rebuttably presumed to have engaged in a general business practice of discharging and administering its compensation obligations in a manner causing injury to those dealing with it.
Upon a second or subsequent finding the administrative director shall refer the matter to the Insurance Commissioner or the Director of Industrial Relations and request that a hearing be conducted to determine whether the certificate of authority, certificate of consent to self-insure, or certificate of consent to administer claims of self-insured employers, as the case may be, shall be revoked.
(e) (f) An insurer, self-insured employer, or third-party administrator may file a written request for a conference with the administrative director within seven days after receipt of the a notice of penalty assessment issued pursuant to subdivisions (a) or (d) , (c) or (d). Within 15 days of the conference, the administrative director shall issue a notice of findings and serve it upon the contesting party by registered or certified mail. Any amount found due by the administrative director shall become due and payable 30 days after receipt of the notice of findings. The 30 day period shall be tolled during any appeal. A writ of mandate may be taken from the findings to the appropriate superior court upon execution by the contesting party of a bond to the state in the principal sum that is double the amount found due and ordered by the administrative director, on the condition that the contesting party shall pay any judgment and costs rendered against it for the amount.
(g) An insurer, self-insured employer, or third-party administrator may file a written request for a hearing before the Workers' Compensation Appeals Board within seven days after receipt of a notice of penalty assessment issued pursuant to subdivision (e) Within 30 days of the hearing, the Appeals Board shall issue findings and orders and serve them upon the contesting party in the manner provided in its rules. Any amount found due by the Appeals Board shall become due and payable 45 days after receipt of the notice of findings. Judicial review of the findings and order shall be had in the manner provided by Article 2 (commencing with section 5950) of Chapter 7 of Part 4 of Division 4 of this code. The 45 day period shall be tolled during appellate proceedings upon execution by the contesting party of a bond to the state in a principal sum that is double the amount found due and ordered by the Appeals Board on the condition that the contesting party shall pay the amount ultimately determined to be due and any costs awarded by an appellate court.
(e) (h) An insurer, self-insured [No other change].
(f) (i) Nothing in this [No other change].
(g) (j) All moneys collected under this section shall be deposited in the State Treasury and credited to the Workplace Health and Safety Revolving Fund Workers' Compensation Administration Revolving Fund.
SECTION 6. Section 4628 of the Labor Code is amended to read:
§4628 (a) Except as provided [No change].
(b) The report shall [No change].
(c) If the initial [No change].
(d) No amount may [No change].
(e) Failure to comply [No change].
(f) Knowing failure to comply with the requirements of this section shall subject the physician to a civil penalty of up to one thousand ($1,000) for each violation to be assessed by a worker's compensation judge or the appeals board. All civil penalties collected under this section shall be deposited in the State Treasury and credited to the Workers' Compensation Administration Revolving Fund.
(g) A physician who [No change].
(h) Knowing failure to [No change].
(i) Any person billing [No change].
(j) The report shall [No change].
(k) The physician shall [No change].

